2017 Fall
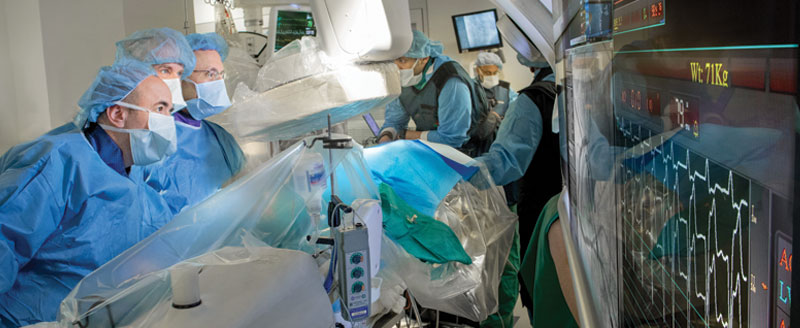
(L to R) Interventional Cardiologists Itsik Ben-Dor, MD, Ronald Waksman, MD, and Lowell Satler, MD, employ an array of structural heart percutaneous devices to tackle degenerative mitral valve disease.
Ever since the success of transcatheter aortic valve replacement (TAVR), MedStar Heart & Vascular Institute’s (MHVI) structural heart specialists have pursued replicating that experience in the mitral valve space. The mitral valve, however, has a unique set of challenges—it changes geometrically during a single cardiac cycle; it is subject to higher closing pressures; and it lacks a reliable native annular anchor to hold a non-surgical replacement.
Less than a decade later, however, MHVI’s efforts are paying off in full.
“There’s been an explosion of new percutaneous devices to repair or replace a leaky mitral valve over the last few years,” says interventional cardiologist Lowell Satler, MD, director of MedStar Washington Hospital Center’s Cardiac Catheterization Lab and a leading figure in understanding and managing structural heart disease. “We now have alternative, and less invasive, options to open surgery.”
In fact, the Edwards Sapien S3 valve, which MedStar Washington Hospital Center tested through the MITRAL trial, just received FDA approval in June as a surgical alternative for high-risk patients with a failing surgical bioprosthetic mitral valve. Other mitral valve trials at MHVI have also demonstrated their efficacy. The MitraClip became the first device to repair degenerative mitral regurgitation, receiving approval from both the FDA and CMS for high surgical risk patients.
“Our experience combining interventional cardiology, cardiac surgery, and advanced imaging proves that we can often use a catheter-based strategy for structural disease as a new alternative to a standard open-chest operation,” Dr. Satler says. “That’s an especially important development for elderly patients who are often already frail and debilitated by co-morbidities, placing them at high or intolerable surgical risk.”









