Cross-Linking Eye Procedure Stops the Progression of Vision Loss
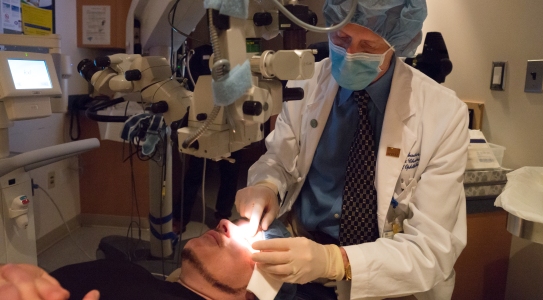
A new procedure that stops the progression of vision loss and the need for a corneal transplant is now available at MedStar Georgetown University Hospital. The procedure is mainly for people with a genetic condition called keratoconus, which causes the thinning and reshaping of the cornea. The weakened corneal structure leads to visual impairment over time. To prevent further vision damage, doctors use the new FDA-approved collagen corneal cross-linking procedure to strengthen the cornea.
“I was lucky because they caught mine early,” says 39-year-old Anthony Philips, who was diagnosed with keratoconus during a work-up appointment for LASIK eye surgery to improve his vision. “A lot of times this condition goes unnoticed.”
Anthony experienced three years of prescription glasses, failed attempts to fit contact lenses, and some double vision episodes before his diagnosis. Test results from the LASIK appointment led to his immediate referral to MedStar Georgetown, where he was a candidate for cross-linking.
“It’s fantastic that we now have the opportunity to help patients with cross-linking,” says Jay Lustbader, MD, chair, Department of Ophthalmology and director of Cornea and Refractive Surgery at MedStar Georgetown. “We can help patients avoid corneal transplantation in a non-invasive way, and it can make a big difference in their life.”
Dr. Lustbader says that any patient who has progressive keratoconus, which can first appear as astigmatism that is getting worse or double vision in one eye, is a candidate for collagen corneal cross-linking.
Cross-Linking: How it Works
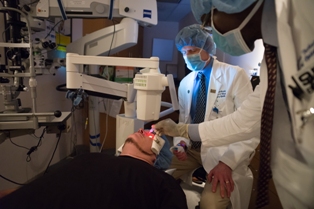 In a one-hour, non-incisional treatment, the MedStar Georgetown Ophthalmology team uses the Avedro KXL Collagen Cross-linking system to reshape the cornea. Patients are given numbing drops for comfort before and during the cross-linking procedure.
In a one-hour, non-incisional treatment, the MedStar Georgetown Ophthalmology team uses the Avedro KXL Collagen Cross-linking system to reshape the cornea. Patients are given numbing drops for comfort before and during the cross-linking procedure.
To strengthen the cornea’s collagen fibers, ophthalmologists use eye drops and the cross-linking system’s ultraviolet light to rebuild the strength of the cornea.
“Patients don’t really feel anything,” says Dr. Lustbader. “While we can prevent more vision loss with cross-linking, there’s also a chance to see vision improvements, by making the cornea more regular in shape.”
After the Procedure
At the end of the procedure, the ophthalmologist places a protective contact lens in the eye and gives sunglasses to the patient. Patients should not rub the eye.
For a few days, patients wear the protective contact lens over their cornea. The contact lens can be worn while sleeping and should only be removed by someone from the Ophthalmology team. Dr. Lustbader says that the cornea surface regenerates in 24-48 hours, like skin. Strengthening of the cornea occurs over several months after the treatment, which stops the progression of vision loss.
After the procedure, some patients might experience minor soreness that can be treated with acetaminophen or other pain medication.
Better Care for Better Vision
“The procedure was painless and recovery was a lot easier than I thought it was going to be! At my last check-up, my doctor noticed that I was already showing great progress and ahead of the game,” says Philips. “This is all still new to me. I had never heard of keratoconus before.”
Although Philips recalls his keratoconus diagnosis as a shocking moment, the condition is very familiar to the Ophthalmology team at MedStar Georgetown.
“We have had many years of experience in treating patients with these conditions, and now we have exciting tools to help us better care for them,” says Dr. Lustbader. “We have the full spectrum of treatment here.”
All corneal surgeons and technicians on the Ophthalmology team have been trained and certified in this new cross-linking procedure since January 2017.
“I want people to know that if you feel like your eye doctor is not getting your prescription right, go somewhere where they have the equipment to get you better answers,” says Philips.
Categories
Media Contact
Marianne Worley
Director of Media Relations
Office: 703-558-1287Pager: 202-405-2824
worleym@gunet.georgetown.edu









