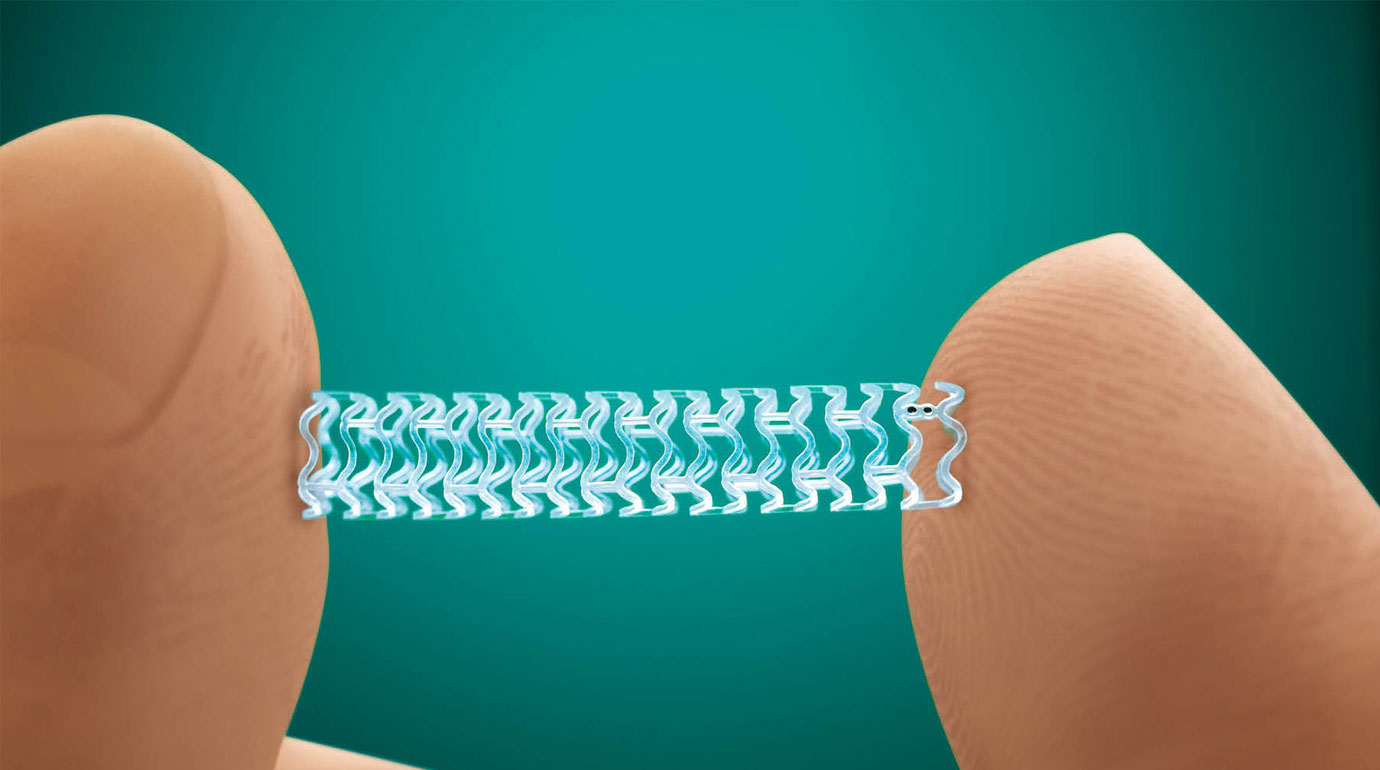
Absorb™ Stent Opens Clogged Arteries, then Gradually Dissolves in the Body
Washington, D.C., August 30, 2016 – A heart stent that slowly dissolves into the body is now available for patients with clogged arteries. MedStar Heart & Vascular Institute became the first in the Baltimore-Washington area to offer the Absorb scaffold, the first bioresorbable stent recently approved by the FDA. MedStar Heart was one of the top enrollers in the pivotal clinical trial that led to the scaffold’s approval.
Currently, MedStar Washington Hospital Center and MedStar Union Memorial Hospital in Baltimore offer the new stent. At the Hospital Center, a man in his 80s became the first patient to receive the dissolvable stent a month after the FDA approval.
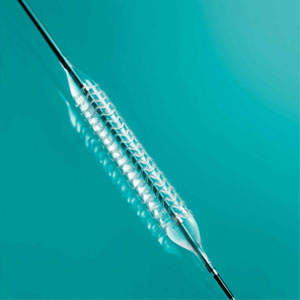 Stents are small scaffolds that prop open a clogged artery to restore blood flow to the heart. Traditionally, they are made of metal and remain permanently inside a patient’s artery. Absorb is made of a naturally dissolving material, similar to dissolving sutures. Absorb gradually dissolves after one year and completely disappears in the body in approximately three years, leaving nothing behind. Only four tiny metallic markers remain in the artery to identify its prior location.
Stents are small scaffolds that prop open a clogged artery to restore blood flow to the heart. Traditionally, they are made of metal and remain permanently inside a patient’s artery. Absorb is made of a naturally dissolving material, similar to dissolving sutures. Absorb gradually dissolves after one year and completely disappears in the body in approximately three years, leaving nothing behind. Only four tiny metallic markers remain in the artery to identify its prior location.
“The Absorb scaffold is a major advancement in the treatment of coronary artery disease that has the potential to affect quality of life and address patients’ desire to leave no metallic stent behind,” said Ron Waksman, MD, director of Cardiovascular Research at MedStar Heart & Vascular Institute, and the principal investigator of the ABSORB III trial. “The fact that no metal material is left in the body allows the vessel to heal itself and reduces adverse side effects of permanent implants.”
However, the new treatment option isn’t for everyone. Patients who received Absorb fared similarly as those receiving a conventional metal stent after one year in the ABSORB study. But heart-related complications were slightly higher with Absorb versus those patients with the metal stent. In addition, patients with very small vessels or those who can’t take blood-thinning medication for long periods are not good candidates.
Dr. Waksman added that the MedStar interventional cardiology team will still rely on traditional types of stents for the majority of the patients with coronary heart disease. A long-term safety assessment on Absorb may take several years.
Categories
Media Contact
So Young Pak
202-877-2748soyoung.pak@medstar.net
Sylvia Ballinger
202-877-7072sylvia.t.ballinger@medstar.net









