TAVR Clinical Trial Provides ‘Strong Signal’ Procedure is Safe for Patients with Low Surgical Mortality Risk
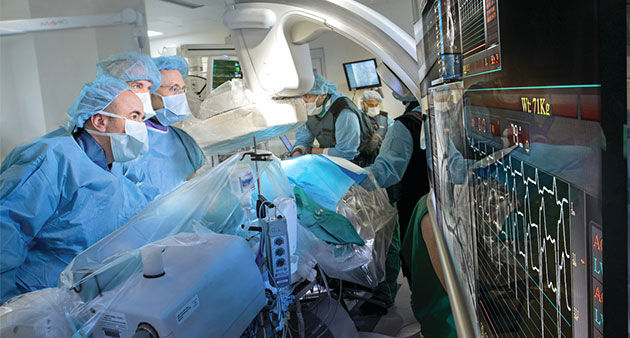
Washington, D.C., September 5, 2018 – Results of a clinical trial using transcatheter aortic valve replacement provided a “strong signal” that it is safe for patients with low surgical risk, potentially helping to open the way for broader use of the minimally invasive procedure, also known as TAVR.
The Low-Risk TAVR trial results, presented at the European Society of Cardiology Congress in late August, showed no deaths or disabling strokes within 30 days of undergoing the procedure for 200 patients with low surgical risk who participated in the study, led by MedStar Heart & Vascular Institute at MedStar Washington Hospital Center.
The results of the trial–the firs-of-its-kind approved by the Food and Drug Administration–were published online in the Journal of the American College of Cardiology.
TAVR is currently approved by the FDA for patients with symptomatic severe aortic stenosis– an abnormal narrowing of the aortic valve in the heart–who are at extreme, high and intermediate risk for death from surgery. Surgical aortic valve replacement, or SAVR is the standard of care for the low-risk population, but the trial results indicate that TAVR in low-risk patients is a safe alternative, with lower complication rates from the procedure.
SAVR involves open heart surgery to replace the valve, while with TAVR, instead of opening the chest, physicians insert a new valve using a catheter threaded into the heart through a small incision in the groin or chest wall.
“The results of the Low-Risk TAVR trial are a strong signal that it is just a matter of time until TAVR is approved for general use with low-risk patients,” said Ron Waksman, MD, director, Cardiovascular Research and Advanced Education, MedStar Heart & Vascular Institute at MedStar Washington Hospital Center, and the study’s principal investigator.
The trial, conducted at 11 medical centers, compared results for the 200 TAVR patients with a control group of 719 patients who underwent SAVR at the same institutions. There were no deaths in the TAVR group at 30 days versus a 1.7 percent mortality rate in the SAVR group. Also, there were no in-hospital strokes in the TAVR group versus a 0.6% stroke rate in the SAVR group.
Dr. Waksman emphasized that the trial was sponsored by the participating investigators, heart teams and centers. The trial was managed by the academic clinical research organization at MedStar Heart & Vascular Institute.
“We are grateful to the FDA for trusting us to be the first to conduct a low-risk TAVR study in the U.S.,” Dr. Waksman said. “We are grateful to all the investigators across the U.S. who were willing to conduct the study at their own expense. They showed exceptional dedication and commitment.”
About MedStar Heart & Vascular Institute:
MedStar Heart & Vascular Institute is a national leader in the research, diagnosis and treatment of cardiovascular disease. A network of 10 hospitals and 150 cardiovascular physicians throughout Maryland, Northern Virginia and the Greater Washington, D.C., region, MedStar Heart also offers a clinical and research alliance with Cleveland Clinic Heart & Vascular Institute, the nation’s #1 heart program. Together, they have forged a relationship of shared expertise to enhance quality, improve safety and increase access to advanced services. MedStar Heart & Vascular Institute was founded at MedStar Washington Hospital Center, home to the Nancy and Harold Zirkin Heart & Vascular Hospital. Opened in July 2016, the hospital ushered in a new era of coordinated, centralized specialty care for patients with even the most complex heart and vascular diagnoses.









