Find care now
If you are experiencing a medical emergency, please call 911 or seek care at an emergency room.
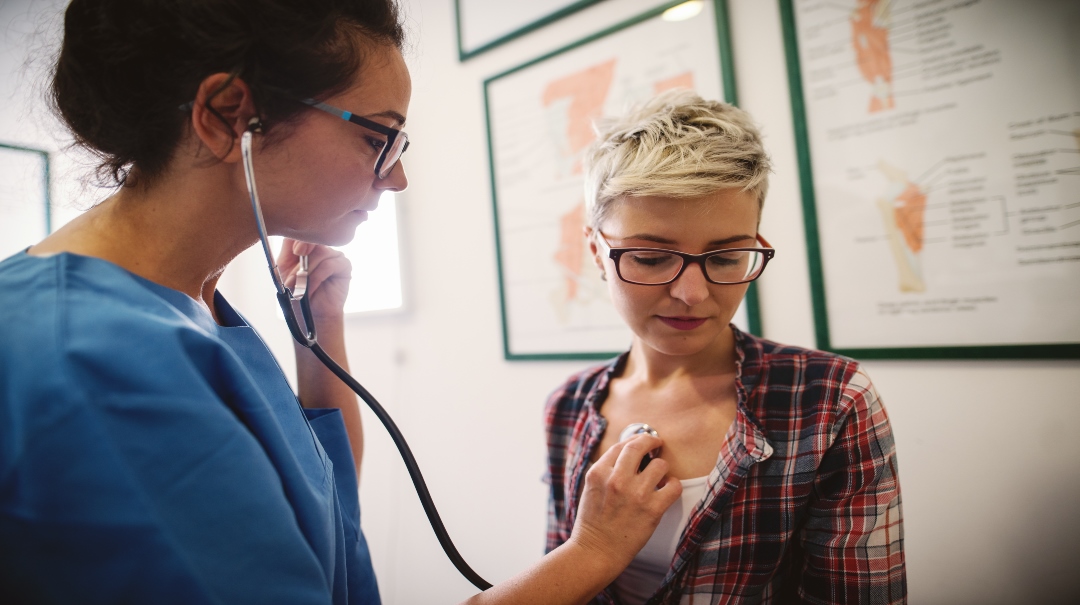
Most of the time, when we talk to patients about dealing with their risk for heart disease, we’re speaking to people in their 50s or older. These patients unfortunately often present after they are feeling bad and need to make changes immediately.
However, when it comes to younger adults—those in their 20s or 30s—it’s often a different story. These patients usually have a family history of heart disease, and either genetic predispositions or lifestyles may have them sitting on risk that could build up for decades, eventually leading to serious heart problems. It can be challenging to take action against heart disease when you might not even notice any problems for 10 or 20 years, but our goal for younger patients is to prevent problems before they ever start.
Warning Signs of Heart Disease in Young Adults
We most often see young adults after they’ve been referred to us by their primary care doctors. They might have gone to the doctor for a regular checkup or some other problem. During that visit, warning signs such as inappropriately high blood pressure or cholesterol can identify an increased risk for developing cardiovascular disease. Sometimes, even when there are no other risk factors, a strong family history of heart disease can identify when someone is at an increased risk for developing heart disease.
Related reading: High Blood Pressure in Young Adults: What Causes It, and How Do We Treat It?
Sometimes, however, the process is driven by the younger patients themselves rather than their doctors. They tell us that their mom or dad had a heart attack in their 30s or 40s, and they want to know what they should be doing so that doesn’t happen to them. In both cases, it’s great when younger adults are proactive about their risk factors for heart disease, as it’s much better to prevent heart issues before they start than it is to treat them after damage has started to occur.
Making Treatment Easier
It's often easier to address heart disease for older people compared to their younger counterparts. Unfortunately, older patients often have developed symptoms of heart disease or have seen a friend or loved one with heart disease, which has led them to the doctor’s office.
In a younger patient with no symptoms, however, they’re much less likely to take a medication that causes unwelcome side effects, such as drowsiness, headaches, increased urination, or nausea (common effects of some medicines). From the young adult’s perspective, this makes sense. They feel fine, they’re not sick, so why take medicine that makes them feel bad?
We have to be more strategic with our treatment plans for young adults. They have to have therapies that are simpler to incorporate into their lives. It’s much easier to make time for a pill taken just once a day versus one that they have to take two, three, or more times in a day. Also, we have to consider medications with minimal side effects so the patients continue to take their medications as directed, rather than skipping doses or stopping treatment.
When it comes to #heartdisease risk, young adults are more likely to stick with treatments that fit into their busy lives. Ask your #cardiologist about medications that are easier to take and have fewer #sideeffects, https://bit.ly/2wjYQJx via @MedStarWHC @NickPaivanas
How We Measure the Effects of Prevention
With older patients, as well as those with active heart disease, it’s obvious when we’re making progress in our treatment regimens. They may experience less pain or shortness of breath, increased energy, and other benefits that are clear to see. However, with a younger adult who may not yet have experienced heart disease symptoms, it’s often harder to see progress. That can make it harder to keep them motivated to continue with their treatment. So we frequently have to take a deeper dive with how we measure our efforts.
Monitoring Bloodwork
Many times, we’ll follow younger patients’ bloodwork more closely to demonstrate the benefits of their treatment, which might not be so obvious otherwise. For example, if a patient has high cholesterol, and we get them on lifestyle changes and cholesterol-lowering medications, I’ll follow their blood cholesterol over several office visits to demonstrate how well they’re doing and how much progress they’ve made over a period of time. That data can provide the gratification and sense of accomplishment a younger adult needs to stay on track with their treatment.
Smartwatches and Fitness Trackers
Seeing data is another great way to help track progress. That’s why I’ve enjoyed seeing smartwatches and fitness trackers become more prevalent in recent years. These devices are a great way to let young adults set and measure goals related to their heart health, such as:
- Heart rate
- Quality of sleep, especially for patients with or at risk of sleep apnea
- Steps taken
- Time active per day
With busy schedules in both work and home lives, many young patients find it difficult to set aside 30, 60, or 90 minutes each day to hit the gym or go for a jog. But if their regular activities allow them to get in about 10,000 steps per day—which has been shown as a reasonable amount for most healthy adults—and if they can track that with their fitness trackers, they can see that they’re still getting their heart rate up and getting the cardiovascular exercise they need each day. Also, the ability to track often can motivate younger adults to have fun healthy competitions with family members, friends, or coworkers on who can get the most steps in, which can only help them with their heart disease risk in the long run.
Prevention of heart disease can have massive positive effects in the life of a young adult—far more than simply reacting to heart disease that has already developed. By living a healthy lifestyle, increasing activity levels, eating right, and not smoking, these patients are avoiding the kind of damage that can build for decades and develop into heart disease. By the time someone develops heart disease, our options are much more limited.
If you have a family history of heart disease, or if you are concerned about your risk, talk to your primary care doctor or a cardiologist and get a complete evaluation. It’s much easier to take action today to prevent heart disease than it is to try to treat it after damage has been done.














