The MedStar Health - Georgetown University Hospital Residency Program in Internal Medicine and Pediatrics
Mission Statement
At MedStar Georgetown Med-Peds, we strive for clinical excellence in an environment that reflects the Jesuit motto of Cura personalis, “care of the whole person.” Our program seeks to recognize the unique gifts, challenges, and needs of each learner and teacher in our community. Residents graduate with the confidence and competence to excel in caring for patients of all ages in both inpatient and outpatient settings. We seek to recruit students with a diverse array of potential career pathways that build upon the common foundations of Internal Medicine and Pediatrics. We are united by a holistic, humanistic approach to patient care whether pursuing a subspecialty, primary care, global health, transitional care, public policy, academic medicine or hospitalist medicine. This aligns seamlessly with our healthcare system whose mission is to serve our patients, those who care for them, and our communities.
Welcome!
Welcome to the MedStar Georgetown Med-Peds Residency Program! We are dedicated to training physicians to be excellent internists and pediatricians. The Med-Peds program at MedStar Georgetown was founded in 1997 by Dr. Stephen Ray Mitchell, a Med-Peds trained Rheumatologist and former Internal Medicine Program Director. Dr. Mitchell’s initial mission was to create an integrated training program which included all the requisite inpatient and specialty rotations as well as a curriculum dedicated to mastering ambulatory care. Dr. Mitchell went on to become the Dean for Medical Education for the Georgetown Medical School where he served as an incredible role model for our medical students and residents and now serves as a Professor Emeritus and continues his love of patient care and teaching, mentoring, and supporting all things Med-Peds.
While Med-Peds training has changed over the last twenty years, the curriculum continues the commitment to training excellence in both Medicine and Pediatric disciplines. Robust training includes inpatient and outpatient domains and prepares residents for a diversity of career goals. Our program continues the commitment a foundation in outpatient care with dedicated “clinic blocks.” These 2-4 week rotations allow our upper-level residents to become proficient in managing acute and chronic medical problems for patients of all ages and provides for continuity of care four our patients. Furthermore, residents learn about the “systems” that enhance efficiency, satisfaction and outcomes in an academic practice. On a larger scale, they develop an understanding of the strengths and weaknesses of the current primary care system. Hopefully some will contribute to the national dialogue about optimal delivery of health care in this country and abroad. The outpatient clinic has a dedicated Med-Peds Faculty group that fosters mentorship and teaching. Our residents graduate with confidence to practice as a hospitalist. Residents interested sub-specialty careers have ample opportunity to rotate with experts in their fields of interest.
As program director, my first goal is to provide our residents with excellent clinical training in both Medicine and Pediatrics. The next priority is to support each resident with educational opportunities and mentorship towards individualized career goals. Our program is richer given the diverse medical interests of our trainees. Whether this passion is for health care policy, advocacy, global health, subspecialty research, quality improvement, education or anything else, I will try to match the resident with the right advisors and experiences. Upon completion of training at MedStar Georgetown, the Med-Peds trained physicians are ready to excel in a wide range of careers.
Sarah T. Deutsch, MD, Program Director
Combined Medicine-Pediatrics Residency Program
Why train here
Program Highlights:
- Outstanding residents from diverse backgrounds
- Emphasis on teaching including morning reports, noon conferences, Argy elective
- Michael Adams Clinician Educator (MACE) Track
- Global Health Track
- Health Policy Elective
- Social Medicine and Health Equity Track
- Georgetown Lombardi Comprehensive Cancer Center, an N.C.I. designated Comprehensive Cancer Center
- N.I.H. Affiliation
- Center for Clinical Bioethics
- Excellent fellowship match and job placement
- MedStar Affiliation – largest health system in the region
- Proximity to downtown D.C. attractions (Kennedy Center, Smithsonian, historic sites)
- Research: Numerous opportunities for research at Georgetown University, Georgetown Lombardi Comprehensive Cancer Center, & NIH as well as the public health sector in DC
- Extraordinary diversity of living and working in DC Metro region. We have colleagues from across the country and around the world caring for people from all over the globe.
- Located in Washington DC with access for Health Policy & rotations at the NIH
- Magnet Nursing – phenomenal nurses with a great collegial relationship
- Access to our Liver Transplant Center, Lombardi as the primary Oncology center, and MedStar’s Heart & Vascular Institute for advanced cardiac therapies – all preeminent in the region
Curriculum
Overview of Residency Program
At MedStar Georgetown University Hospital, our Med-Peds trained faculty are accessible and dedicated to resident education and clinical teaching. Our program directors seek resident feedback regularly and work hard to make Georgetown Med-Peds an unbeatable training experience.
Residents benefit from seamless integration into our parent programs, but maintain a unique identity as Med-Peds residents in a smaller, close-knit Med-Peds “family.” Both parent departments have consistently demonstrated support and regard for Med-Peds and our residents, and we feel equally engaged in the academic and social communities of both parent departments.
Overall Program Goals
The goal of the Med‐Peds residency training program at the MedStar Georgetown University Hospital is to produce physicians who have developed the competencies to function as independent internists and pediatricians who care for adults and children of all ages.
Objective of the Program
The Med‐Peds residency training program at MedStar Georgetown University Hospital has been designed to enable residents upon completion of the program to be able to:
- Apply established and evolving knowledge in the clinical and epidemiological sciences related to medicine and pediatrics as well as related knowledge in the social‐behavioral sciences to their care of child and adolescent patients. (Medical Knowledge)
- Provide compassionate, appropriate, and effective patient care by:
- Using data about a patient (history, physical examination, laboratory and imaging studies) along with medical knowledge to create a differential diagnosis, plan for further evaluation, and comprehensively manage patients with a variety of disorders. (Patient Care)
- Developing a relationship with patients and their families in which health care needs are identified and addressed collaboratively in the context of the patient as a whole person. (Interpersonal and Communication Skills)
- Improve the patient care that they provide by continuously assessing their performance, incorporating feedback and pursuing learning related to improvement opportunities. (Practice‐based Learning and Improvement)
- Function effectively with the system of health care beyond the clinical encounter to call effectively on additional resources to provide optimal health care for patients with a variety of disorders. (Systems‐based Practice)
- Conduct their professional life in accordance with the expectations of the profession of medicine and society, manifested through a commitment to carrying out professional responsibilities, adherence to ethical principles, and sensitivity to patients of diverse backgrounds. (Professionalism)
- Pursue career in medicine caring for children and adults as a generalist or a sub‐specialist and seek to make an impact as a leader in the medical field improving the delivery of health care in a variety of venues including general medicine, subspecialty medicine, population medicine, health policy, biomedical research, or international health medicine.
Sample Schedule
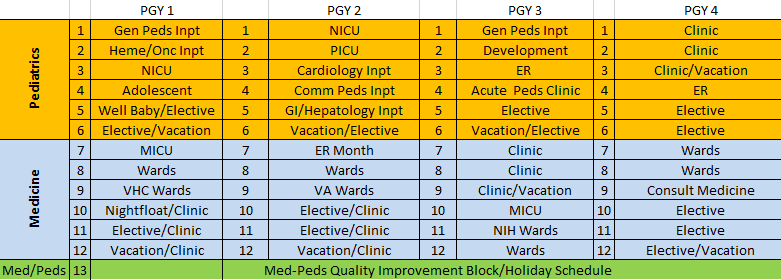
Our program rotates every 3 months between Medicine and Pediatric services. There are 13 rotation blocks each year - this allows for a Med-Peds specific Quality Improvement Block in December/January. Intern year is 12 months.
Continuity Clinic
Residents are provided with strong ambulatory training in both Internal Medicine and Pediatrics, at our Med-Peds continuity clinic which is supervised exclusively by Med-Peds trained faculty. Our clinic moved to a new, freshly renovated location less than a mile from the main hospital in June of 2022. The space was designed to optimize clinic flow and the patient experience. Our entire health care system uses the Cerner EMR which allows for coordination of care across the multiple subspecialty practices and hospitals in the Medstar network. The Med-Peds clinic also functions as a “home away from home” for our residents who look forward to reuniting with peers during their continuity clinic sessions. We have an ambulatory curriculum that includes 100 outpatient topics that repeat every 2 years. The pre-clinic conference is a mixture of case -based discussions led by faculty AND board review questions.
Our Internal Medicine program has adopted a “X + Y” scheduling system, while Pediatrics maintains a weekly continuity clinic. The Med-Peds residents follow this alternating structure. They attend weekly clinic when on pediatric rotations and longitudinal blocks when on medicine. Continuity blocks include didactic sessions with categorical residents, as well as subspecialty experience. A sample schedule is listed below:
| Day | AM | PM |
| Monday | Subspecialty Clinic | Continuity Clinic |
| Tuesday | Ambulatory Didactics | Pre-Clinic Conference Continuity Clinic |
| Wednesday | Continuity Clinic | Administrative Time |
| Thursday | Continuity Clinic | Medicine Grand Rounds Subspecialty Clinic |
| Friday | Pediatric Grand Rounds Continuity Clinic |
Continuity Clinic |
The third and fourth year schedules include additional ambulatory time (three months per year) in the MedStar Georgetown Med-Peds clinic. Whether they are aspiring to a clinical career in primary care, as a hospitalist OR subspecialist, understanding how medical care is delivered in an outpatient setting is a critically important skill that our residents master. tur residents are experts in managing We aim to align the “subspecialty experience” with the professional and academic goals of the trainee. Some need the time for research, or desire exposure to community healthy sites. In addition to the usual medicine subspecialties, we’ve arranged rotations in family planning, sports medicine, school-based clinics, lactation, physical therapy, FQHCs, local private practices, ENT and with the DC DOH.
Residents on the Med-Peds ambulatory block are expected to perform thorough evaluations of patients in the office, attend conferences and lectures, and complete outside reading and self-study. During the rotation, residents are expected to become knowledgeable and proficient in the basics of preventative and general internal medicine and pediatrics, as well as common urgent care issues arising in the office.
The clinic is located at 2233 Wisconsin Avenue and is open from 8:30 am to 5 pm Monday through Friday. Residents are asked to evaluate patients and then present their findings, assessment, and plan to the designated Med-Peds Preceptor. The preceptor then sees the patient to verify exam findings for all intern encounters in the first 6 months of training. Subsequently, faculty may opt not to see certain patients if they concur with the resident’s diagnostic impression and plan of care. Faculty are ALWAYS amenable to seeing any patient when requested by the resident or patient/parent.
Training Locations
- MedStar Georgetown University Hospital- Core training site
- Inova Fairfax - Pediatric ER, PICU, Heme/Onc, General Pediatric Wards
- Virginia Hospital Center - Newborn Nursery and Medicine Wards
- Shady Grove Hospital - Pediatric ER
- Children’s National Medical Center - Pediatric Wards, PICU, Electives
- The National Institutes of Health - Medicine Wards and Electives
- Veterans Affairs Medical Center – Medicine Wards and Electives
- MedStar Washington Hospital Center- Medicine Cardiology and CCU
Contact Us
Medicine-Pediatrics Residency
MedStar Georgetown University Department of Medicine
Pasquerilla Healthcare Center, 5th Floor
3800 Reservoir Rd, NW
Washington, DC 20007
Please feel free to contact us with questions regarding the Medicine-Pediatrics Residency Program.
Amber Weller
Internal Medicine & Pediatrics Residency Administrator
Amber.R.Weller@gunet.georgetown.edu
Ph: 202-444-0809
2025-2026 Medicine-Pediatrics Chief Residents
Devin Boe, Md, PhD, Vincent Cendan, MD, Tyler Clay, MD and Grace Hunt, MD
GUHMedPedsChiefs@gunet.Georgetown.edu
Application Information
Requirements
- ERAS common application form
- NRMP #: 1801700C0
- Personal Statement
- CV
- Dean’s Letter
- 3-4 Letters of Recommendation
- Include letters from faculty who can comment on your clinical skills in Internal Medicine and Pediatrics. Departmental Letters of support are encouraged, but not required.
- Medical School Transcript
- USMLE/COMLEX Results- Step 1 and Step 2 when available
2025-2026 Medicine-Pediatrics interview dates
- October 21, 2025
- November 4, 2025
- November 11, 2025
- November 18, 2025
- December 2, 2025
- December 9, 2025
- December 16, 2025
- January 6, 2026
This year, interviews will be entirely virtual and will be one day in duration. In addition, our program will be offering an optional one-hour virtual event the night before your interview with our current Residents. Our program will be offering second looks this interview season.
Application Deadline: November 15
Register for MyERAS for Residency:
https://students-residents.aamc.org/register-myeras/register-myeras-residency
For Canadian Applicants:
https://www.carms.ca/the-match/application-to-the-us-eras/
For International Applicants:
https://www.ecfmg.org/eras/applicants-eligibility.html
Visa Policy
J-visas may be sponsored; however, applicants may be required to assume the costs of preparing and obtaining the appropriate documents needed for sponsorship.
Georgetown University Medical Center is an equal opportunity employer.









