Research publications
-
Dixit, R. A., Ratwani, R. M., Bishop, J. A., Schulman, K., Sharp, C., Palakanis, K., & Booker, E. (2022). The impact of expanded telehealth availability on primary care utilization. npj Digital Medicine, 5(1), 141.
-
Boxley, C., Dixit, R., Katharine, A., Anderson, R., Ratwani, R. M., & Booker, E. (in press). The impact of COVID-19 on primary care accessibility and the role of telehealth for patients with chronic conditions. Health Policy and Technology, 12(3).
-
Apathy, N.C., Dixit, R., Boxley, C., Adams, K., Booker, E., Ratwani, R.M. (in press). Association of visit characteristics with variation in telemedicine use. JAMA Network Open.
Principal investigator perspective
"While we expected to see variability in telehealth use in primary care, we were interested to learn that those patients with chronic illness and frequent primary care needs consistently replaced one to two visits per year with a telehealth visit. This finding underscores our entry into a new era of chronic care, as telehealth helps providers increase access and care continuity for patients who need it most. Given the evidence that telehealth has expanded our care capabilities, we believe federal and state legislation and regulations should continue to protect telehealth access."
- Ethan Booker, MD, study co-author, co-principal investigator for both grants, and chief medical officer of telehealth for MedStar Health
Learn more in the study and press release.
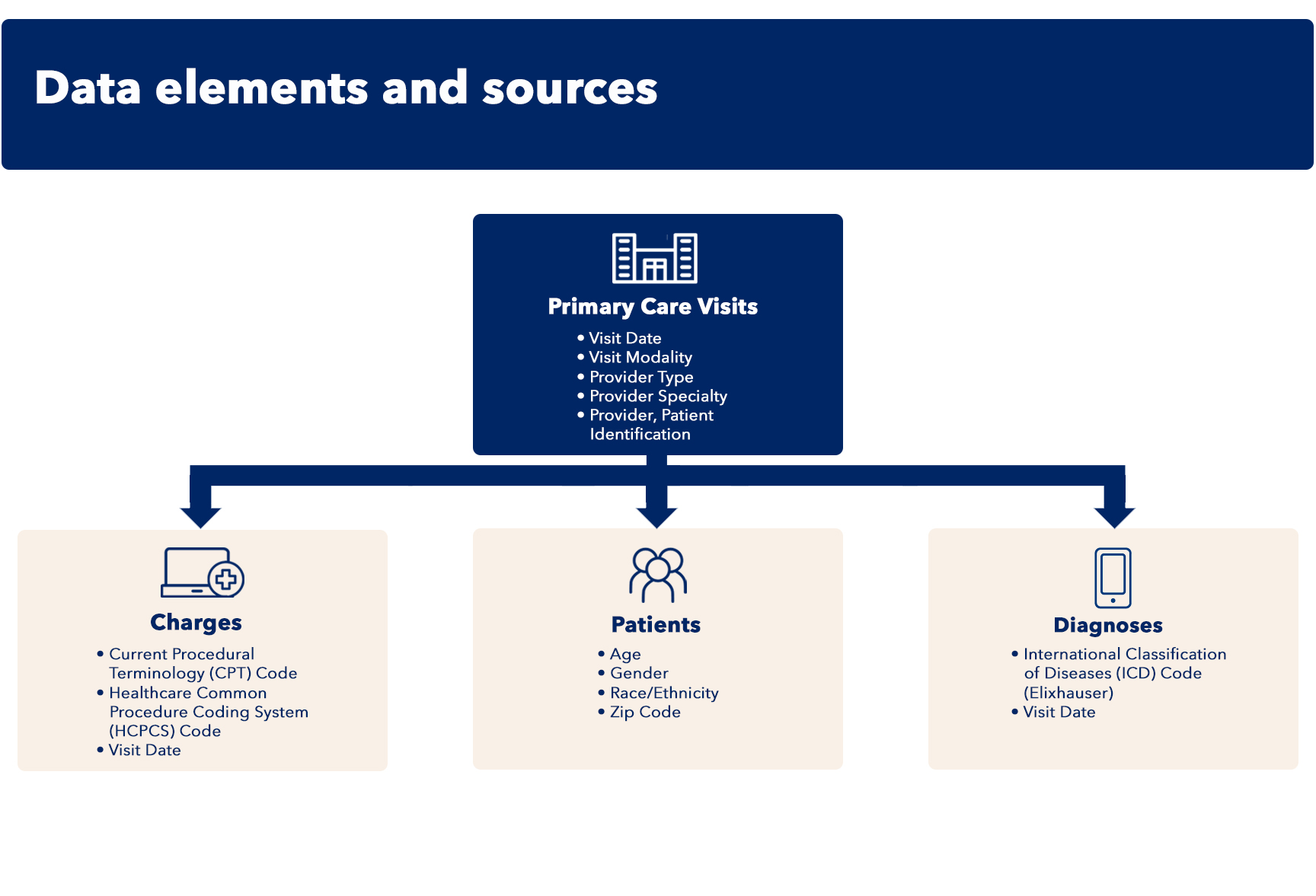
Primary care studies: Our exceptional dataset and data model
Together, we have built and are analyzing a dataset of 1.2 million patients (more than 5 million encounters) who sought primary care between January 1, 2018 to December 31, 2021 from various healthcare systems. Our primary study leveraging this full dataset will be the largest of its kind.
Data element examples:
-
Visit modality: Office, phone, video
-
Race/ethnicity: Asian, Black, Latino, Other/Unknown, and White
-
Diagnoses/conditions (most common): Cardiac arrythmias, chronic pulmonary disease, depression, diabetes (uncomplicated), hypertension (uncomplicated), hypothyroidism, obesity
-
CPT code categories/services: Evaluation and management, medicine, pathology and laboratory, radiology, and surgery
Patient safety learning laboratory: Areas to explore
Our co-principal investigators identified “the four Ps” of initial research possibilities to provide more insight into their vision for this work and will remain open to what the researchers learn from the data:
Proactive opportunities to advance safety and health through telehealth
Our team will reach beyond the study of existing ways to enhance the safe use of telehealth to consider how to leverage telehealth technology to proactively increase safety, such as reviewing a patient’s medicine cabinet during a video visit.
Process optimizations that can complement technology enhancements
Our experts shaping this work bring an important blend of clinical, technical, human factors, systems engineering, and other knowledge to consider how process also ties closely to safety progress, like the ability to support continued care referrals surrounding visits.
Personalization of telehealth technology for both safety and health equity
Our research findings underscore the critical need to protect access to a variety of telehealth tools to ensure safety and health equity, including video, phone, and other unique connected care tools, such as chatbots. This is especially important to our most vulnerable populations.
Provider wellbeing prioritization within increasingly connected care
Our team is also uniquely positioned to study how increasingly connected care might tie to provider wellbeing and patient safety. New realities, such as an enormous increase in patient portal messages, for example, potentially result in new after hours work for providers.
Principal investigator perspective
“Our initial research demonstrates that telehealth is delivering on its promise to provide accessible and effective care. Thanks to the continued support of AHRQ, we will advance patient safety nationally by studying and scaling telehealth as a proactive safety tool while also enhancing its safe use within the diverse communities served by connected care.”
- Raj Ratwani, PhD, co-principal investigator for both grants, vice president of scientific affairs for the MedStar Health Research Institute, and director of the MedStar Health National Center for Human Factors in Healthcare.
Learn more in the related press release.
Speaking engagements and strategic meetings
Our teams have been sharing initial insights directly with policymakers—from the Congressional Budget Office to the Office of the Assistant Secretary for Health—and in other more public forums. Here are some examples:
-
Becker's Health IT + Digital Health + RCM Annual Meeting, “Inside the Culture Transformation of Elite Tech-Enabled Care Teams”
-
Listen to Ethan Booker, MD on the Becker's Healthcare Podcast
-
Read more about related topics via Becker's, “How are other systems breaking down data silos? 35 leaders share”
-
-
National Committee for Quality Assurance (NCQA), How telehealth supports quality improvement and how it is measured, "Telehealthier: Improving Access and Increasing Care"
-
Human Factors and Ergonomics Society (HFES), 2022 International Symposium, “Socio-technical Factors for Telehealth Success”
-
Human Factors and Ergonomics Society (HFES), 2021 International Symposium, “Human Factors and Telehealth: Opportunities for Research, Design, and Implementation”
-
U.S. House of Representatives Committee on Energy and Commerce, Subcommittee on Health, “Hearing Concerning the Future of Telehealth: How COVID-19 is Changing the Delivery of Virtual Care”
Stay connected
Questions about our work or how to get involved? Contact us here.
Page last updated: 12/5/23