The MedStar Health—MedStar Georgetown University Hospital/Washington Hospital Center Ophthalmology Residency Program
Chairman: Jay M. Lustbader, MD
Program Director: Aruoriwo Oboh-Weilke, MD
The MedStar Georgetown University Hospital/Washington Hospital Center ophthalmology residency program is a fully accredited, four-year integrated program that combines dedicated and expert clinicians/educators, modern technology, and experience in resident education to present a challenging and rewarding training opportunity.
Established in July 2002 from the integration of two independently excellent and longstanding programs, this residency provides trainees with access to a large teaching faculty, a broad clinical and surgical experience, and a very diverse patient population. Training is scheduled at a variety of institutions optimizing residents’ exposure to a wide range of ocular conditions and culminates in a unique opportunity for senior residents to assume charge of their own clinic practices.
Washington National Eye Center, Inc. (WNEC) at MedStar Washington Hospital Center (MWHC) is the primary training venue for the residency program. WNEC is one of the largest and most complete ophthalmology clinics in the metropolitan Washington area, including facilities for laser therapy, ultrasonography, digital fluorescein angiography, visual fields, OCT, Pentacam, auto refraction, and corneal topography, in addition to fully-equipped examination and minor procedure rooms. Its vitreoretinal service is the busiest in the Washington, D.C., area and one of the largest in the United States.
Residents complement their training at WNEC with major rotations at MedStar Georgetown University Hospital (MGUH), MedStar St. Mary’s Hospital, the DC Veterans Affairs Medical Center (VA), Walter Reed National Military Medical Center (WRB), INOVA Fairfax Hospital (FFX), and Children's National Medical Center (CNMC). Training at these locations serves to broaden their clinical and surgical experiences and allows them to explore areas of subspecialty training.
Affiliates
-
Washington National Eye Center, Inc. at MedStar Washington Hospital Center
110 Irving Street, NW, Suite 1A-19, Washington, D.C., 20010Jay M. Lustbader, MD, Chairman
Stacy Y. Bang, MD, Chief, Comprehensive Ophthalmology and Clinic DirectorThe Washington National Eye Center (WNEC) at MedStar Washington Hospital Center (MWHC) is a comprehensive ophthalmology facility, offering a wide selection of diagnostic and treatment options, including laser therapy; ultrasonography; fluorescein angiography; visual fields; pachymetry, corneal topography and much more. In addition to the general ophthalmology clinic, the WNEC offers a range of specialty clinics, including retina, glaucoma, cornea, ocular motility, low vision, uveitis, oculoplastics, and neuro-ophthalmology.
All examination rooms at WNEC are fully equipped. MWHC has an operating room dedicated to eye surgery, fully equipped and staffed by highly skilled nurses, technicians and other personnel. Surgical services are supported by excellent admitting, pre-operative testing, and recovery teams. Ophthalmology attending physicians supervise residents in the clinics, in the operating room, as well as on-call for after-hours emergencies.
WNEC/MWHC Annual Statistics:
- 20,000+ patient procedures
- 1,200 total surgeries
- 700 resident surgeries
- 13,000+ cataract/general evaluations
- 5,000+ glaucoma evaluations
- 3,000+ retina evaluations
Core Faculty:
- Abdullah Abou-Samra, MD, Senior Retina Fellow
- Andrew J. Adelson, MD, Glaucoma, Low Vision, Comprehensive
- Monica Allen, MD, Glaucoma, Comprehensive
- Frank S. Ashburn III, MD, Glaucoma
- Stacy Y. Bang, MD, Cornea
- Michael D. Baum, MD, Comprehensive
- Salim I. Butrus, MD, Cornea, Comprehensive
- Rosan Y. Choi, MD, Comprehensive, Research Chief
- Jordana Fein, MD, Retina
- Reena A. Garg, MD, Glaucoma, Comprehensive
- Alice T. Gasch, MD, Uveitis
- Lauren Z. Gavaris, MD, Oculoplastics
- Maxwell A. Helfgott, MD, Comprehensive
- Jason Mingyi Huang, MD, Retina
- Sarah Kamal, MD, Senior Retina Fellow
- Aziz Khanifar, MD, Retina
- Martin P. Kolsky, MD, Neuro-Ophthalmology
- Michael M. Lai, MD, PhD, Retina
- Jay M. Lustbader, MD, Cornea, Refractive, Comprehensive
- Mariam Mathai, MD, Retina
- Viraj Mehta, MD, Oculoplastics
- Alexander Melamud, MD, Retina and Fellowship Director
- Nima Moainie, MD, Comprehensive, Laser Surgery
- Meghan G. Moroux, MD, Cornea, Comprehensive
- Narieman A. Nik, MD, Oculoplastics
- Aruoriwo Oboh-Weilke, MD, Cornea
- Benjamin Osborne, MD, Neuro-Ophthalmology
- Arnold Oshinsky, MD, Comprehensive
- Anna Park, MD, Comprehensive
- Arthur L. Schwartz, MD, Glaucoma
- Justin Shortell, MD, Glaucoma, Comprehensive
- Namratha Turlapati, MD, Ocular Motility, Comprehensive
- Jacquelyn Weber, MD, Cornea, Comprehensive, Wellness Chief
- Howard S. Weiss, MD, Glaucoma
- Norma L. Zapata-de-Perez, MD, Comprehensive, Safety Officer
-
MedStar Georgetown University Hospital
3800 Reservoir Road, NW, PHC-LL, Washington, DC 20007Jay M. Lustbader, MD, Chairman
Training at MedStar Georgetown University Hospital offers PGY2 and PGY3 residents experience in a more “private-practice” like environment. The hospital’s core of full-time and part-time faculty share their clinical expertise with residents as they participate in the diagnosis and management of ocular conditions not typically encountered in urban clinics, such as age-related macular degeneration, angle-closure glaucoma, intraocular tumors, and cosmetic oculoplastics in addition to a robust contact lens service. The residents also direct, with full faculty supervision, the inpatient consultation and eye emergency services for MGUH.
On a limited basis, residents work in the private offices of attending staff whose patient populations offer unusual educational opportunities. There is a weekly ocular pathology session in which residents work directly with an ophthalmic pathologist in the gross and microscopic examination of surgical specimens. Residents seeking research experience are introduced to the basic science faculty at Georgetown University.
Core Faculty:
- Neal Adams, MD, Electrophysiology
- Jay M. Lustbader, MD, Cornea and Refractive, Comprehensive
- Toufic Melki, MD, Retina
- Teresa Narayan, OD, Optometry and Contact Lens
- Aruoriwo Oboh-Weilke, MD, Cornea, Comprehensive, Medical Student Educator
- Benjamin Osborne, MD, Neuro-Ophthalmology
- Sina Sabet, MD, Ocular Pathology
- Namratha Turlapati, MD, Pediatric Ophthalmology
- David G. Wagner, MD, Retina
- Deborah Wilson-Umanzor, MD, Glaucoma, Comprehensive
-
INOVA Fairfax Hospital
3299 Woodburn Road, #150, Annandale, VA 22003Tofik M. Ali, MD, Site Director
Since its inception in 1974, the ophthalmology service at INOVA Fairfax Hospital (FFX) has been affiliated with the MedStar Georgetown/MedStar Washington ophthalmology teaching program.
Rotations at FFX occur in the PGY3 and PGY4 years of residency. PGY4 residents work at the Hospital full-time for four months; they spend three days per week in the ophthalmology clinic and one and a half days in the operating room. PGY3 year residents spend 1-2 days per week for 2 months at FFX, seeing patients in the clinic and performing non-complex cataract surgeries.
Along with experience in general ophthalmology, the rotation offers extensive subspecialty experience. Residents work with retina specialists during the weekly retina clinics; patients requiring laser procedures are served on-site in the outpatient area of the hospital’s operating rooms. Also, residents are supervised by the hospital’s staff of glaucoma specialists as they evaluate glaucoma patients and participate in glaucoma-related surgeries. Neuro-ophthalmology and oculoplastic clinics are held once a month. Clinic patients requiring cataract surgeries are scheduled during the block time reserved for resident cases.
Core Faculty:
- Tofik Ali, MD, Cornea, Comprehensive
- Mark D. Falls, MD, Comprehensive
- Jordana G. Fein, MD, Retina
- Julie F. Leigh, MD, Uveitis
- Emily Y. Morin, MD, Cornea, Comprehensive
- Anh Nguyen, MD, Cornea, Refractive, Comprehensive
- Juliana Y. Park, MD, Cornea, Comprehensive
- David L. Parver, MD, Retina
- Bella Patnaik, MD, Cornea, Refractive, Comprehensive
- Muhammad Wesam Silk, MD, Cornea, Comprehensive
-
Washington, D.C., Veterans Affairs Medical Center
50 Irving Street, NW, Ophthalmology Section, Washington, DC 20422Soo Y. Shin, MD, Chief
Under the guidance of excellent faculty at the Washington DC Veterans Affairs Medical Center (VA), residents gain experience in the management and treatment of various ocular conditions. During this rotation, residents see 10-18 patients per day in the clinic. PGY3 residents operate one morning a week and attend oculoplastic surgery once per week. By the end of their 4-month rotation, PGY3 residents have performed an average of 15 cataract extractions as primary surgeon. PGY4 residents operate one to two mornings a week; one of these sessions is dedicated to retina. During their 3-month rotation, senior residents perform 40-50 cataract extractions as primary surgeon. All rotating residents are trained on the Eyesi Anterior Segment Surgery Simulator.
Regularly scheduled daily and subspecialty clinics at the VA offer valuable opportunities for specialized training. Residents have the opportunity to work with corneal specialists, retinologists, glaucoma specialists and oculoplastic surgeons as they attend clinic and perform surgeries.
Core Faculty:
- Sameer I. Ahmad, MD, Glaucoma
- Rosalie L. Bair, MD, Oculoplastics
- Cyrus A. Golshani, MD, Medical Retina
- Julie G. Gutmark, MD, Cornea, Comprehensive
- Michele P. Maiberger, MD, Comprehensive
- Tamer N. Mansour, MD, Oculoplastics
- Arnold L. Oshinsky, MD, Comprehensive
- Soo Y. Shin, MD, Cornea, Comprehensive
- David G. Wagner, MD, Retina
- Deborah Y. Wilson-Umanzor, MD, Glaucoma
-
MedStar St. Mary’s Hospital
2550 Point Lookout Road, Leonardtown, MD 20650Aruoriwo Oboh-Weilke, MD, Interim Chief
The ophthalmology service at MedStar St. Mary’s Hospital (MSMH) serves the entire southern Maryland area, including military bases, military contractors, agricultural enterprise, aquacultural enterprise and a large underserved population.
Rotations at MSMH occur in the PGY4 year. Senior residents work at the Hospital and the nearby outpatient clinic full-time for two months; they spend three days per week in the ophthalmology clinic and one and a half days in the operating room.
Along with experience in general ophthalmology, the rotation offers subspecialty experience as well. Clinic patients requiring cataract surgeries are scheduled during the block time reserved for resident cases.Core Faculty:
- Mark Gonzalez, MD, Comprehensive
- Aruoriwo Oboh-Weilke, MD, Cornea, Comprehensive
- Walter Wang, MD, Glaucoma
-
Walter Reed National Military Medical Center
8901 Rockville Pike, Bethesda, MD 20889Rachel M. Lieberman, MD, Site Director
At Walter Reed National Military Medical Center (WRB) in Bethesda, Maryland, PGY2 residents see patients in a large general ophthalmology setting during a two-month rotation. There is extensive full-time sub-specialty supervision, including an intensive glaucoma and retina experience, as well as regularly-scheduled didactics.
Core Faculty:
- T. Benjamin Abelman, MD, Neuro-Ophthalmology
- Brad Ballard, MD, Pediatric Ophthalmology
- Kevin Broderick, MD, Retina
- Jonathan Buttram, MD, Oculoplastics
- Eva Chou, MD, Oculoplastics
- Matthew Debiec, MD, Retina and Chief
- Okezie Igboeli, MD, Cornea and Refractive
- Grant Justin, MD, Retina
- Christiaan Kroesen, MD, Comprehensive
- Jason Lewis, MD, Oculoplastics
- Rachel Lieberman, MD, Comprehensive
- Morohunranti Ogunotye-Ouma, MD, Glaucoma
- Joseph Pasternak, MD, Cornea and Refractive
-
Children's National Medical Center
111 Michigan Avenue, NW, Washington, DC 20010William P. Madigan, MD, Chairman
Residents in their second year receive an in-depth introduction to pediatric ophthalmology during their two-month rotation through Children’s National Medical Center (CNMC). During this rotation, residents perform ocular muscle surgery and assist on other surgical cases, all under the direct supervision of subspecialty-trained ophthalmologists. In addition to surgery involving ocular motility, residents experience a wide variety of interesting pediatric ophthalmic diseases and conditions.
Core Faculty:
- Marlet Bazemore, MD, MPH, Pediatric Ophthalmology & Strabismus
- Richard Birdsong, MD, Pediatric Ophthalmology & Strabismus
- Brian P. Brooks, MD, PhD, Ophthalmic Genetics
- Salim I. Butrus, MD, Cornea
- William F. Deegan, MD, Retinal Oncology
- Lauren Gavaris, MD, Oculoplastics
- Todd Goodglick, MD, Neuro-Ophthalmology, Oculoplastics and Orbit
- Malack Hamade, MD, Pediatric Ophthalmology and Strabismus
- Claudia Hooten, MD, Retina
- Laryssa Huryn, MD, Ophthalmic Genetics
- Aziz Khanifar, MD, Retina
- Laura Kueny, MD, Pediatric Ophthalmology and Strabismus
- William P. Madigan, MD, Pediatric Ophthalmology & Strabismus and Chairman
- Narieman A. Nik, MD, Oculoplastics
- Reginald J. Sanders, MD, Retina
- Jonathan Taylormoore, MD, Pediatric Ophthalmology & Strabismus
- Gonzalo Vicente, MD, Pediatric Ophthalmology & Strabismus
Why train here
Our residency is structured as a mix of resident-run and attending clinics—a learning environment where residents gain both surgical skills and confidence in their clinical decision making.
Our six teaching locations in and around Washington, D.C., also provide exposure to varied patient populations. The faculty presents didactic lectures to cover both basic science and clinical topics as well as formal wet labs, simulations, and practice-based learning.
The pride of our program is our resident-run clinic at the Washington National Eye Center of MedStar Washington Hospital Center, our residency’s primary home. It is one of the largest and most complete ophthalmology clinics in the metropolitan Washington, D.C., area and its vitreoretinal service is one of the largest in the United States.
The clinic is fully equipped with laser therapy, ultrasonography, digital fluorescein angiography, visual fields, OCT, Pentacam, auto refraction, and corneal topography, in addition to fully equipped examination and minor procedure rooms.
Residents complement their training with major rotations at MedStar Georgetown University Hospital, the D.C. Veterans Affairs Medical Center, INOVA Fairfax Hospital, and Children’s National Medical Center. This exposure broadens clinical and surgical experience and allow the opportunity to explore areas of subspecialty training.
In collaboration with the Retina Group of Washington's fellowship program, our vitreoretinal service is the busiest in the Washington, D.C., area and one of the largest in the United States. Providing a rich experience in urban ophthalmology, MWHC also provides incredible exposure to ocular trauma as the largest Level 1 trauma center for Washington, D.C.
This diversity in instruction, patient population and technology prepares graduates to manage ophthalmic complaints in any setting.
By the time our residents interview for fellowships or private practice positions, they are prepared to impress future instructors, mentors, and colleagues with an excellent fund of knowledge, excellent comprehensive and subspecialty clinical and surgical experience and an excellent portfolio of accomplishments in research, customer satisfaction, process improvement, humanitarianism, and program and national examinations.
Our residents’ written and oral board exam pass rate is well above the national average, and they have succeeded in matching into top fellowships or joining preferred practices all over the country.
Program Highlights:
- Fully accredited by the ACGME
- The only integrated ophthalmology program in Washington, D.C.,
- Washington National Eye Center at MedStar Washington Hospital Center rotations are rich with pathology, trauma, and opportunities for procedures
- In-clinic phaco wet lab at WHC and Eyesi Virtual reality surgical simulator at the VA location
- Fellowship match
Curriculum
Introduction
The principal objective of the MedStar Georgetown University Hospital/MedStar Washington Hospital Center ophthalmology residency program is to produce a skilled ophthalmologist who adheres to the highest professional and ethical standards. The model graduate of this program is an efficient and productive practitioner, who is actively involved in clinical research, either for publication or practice outcomes analysis; who practices with the confidence, compassion, and efficacy of someone with a depth and breadth of the current knowledge in their field; who is aware of their leadership responsibilities and stewardship of their profession, community, and specialty; and finally, someone who understands the necessity and value of continuous learning, adaptation, and inquiry. This is accomplished 1) by ensuring that training is thorough and comprehensive, leading to certification of residency graduates by the American Board of Ophthalmology, 2) by maintaining high professional, educational and ethical standards, 3) by assuring a high level of care for all patients, and 4) by promoting investigative and scientific research.
To help achieve these aims, goals and objectives for each assignment at each educational level have been developed. These Goals and Objectives are competency-based and are distributed to residents and faculty annually, in electronic form.
Curriculum Goals and Objectives
The core principles of the curriculum are based on the integration of the Accreditation Council for Graduate Medical Education (ACGME) Milestones into resident education and evaluation. Within the Milestones lie six competencies, emphasized at all levels of training:
-
Patient care
Residents must be able to provide patient care that is compassionate, appropriate, and effective for the treatment of health problems and the promotion of health. Residents must demonstrate competence in patient care, including: evaluating and assessing preoperative ophthalmic and general medical indications for surgery and surgical risks and benefits, developing intraoperative skills, managing systemic and ocular complications that may be associated with surgery and anesthesia, obtaining informed consent, performing ophthalmic procedures as primary surgeon (including cataract, strabismus, cornea, glaucoma, glaucoma laser, retina/vitreous, oculoplastics/orbit, refractive, and globe trauma), providing acute and long term postoperative care, and using local and general anesthetics. -
Professionalism
Residents must demonstrate a commitment to carrying out professional responsibilities and an adherence to ethical principles. Residents are expected to demonstrate:
- Compassion, integrity, and respect for others;
- Responsiveness to patient needs that supersedes self interest;
- Respect for patient privacy and autonomy;
- Accountability to patients, society and the profession;
- Sensitivity and responsiveness to a diverse patient population including, but not limited to, diversity in gender, age, culture, race, religion, disabilities, and sexual orientation.
-
Systems-based Practice
Residents must demonstrate an awareness of and responsiveness to the larger context and system of health care, as well as the ability to call effectively on other resources in the system to provide optimal health care.
Residents are expected to:- Work effectively in various health care delivery settings and systems relevant to their clinical specialty;
- Coordinate patient care within the health care system relevant to their clinical specialty;
- Incorporate considerations of cost awareness and risk-benefit analysis in patient and/or population-based care as appropriate;
- Advocate for quality patient care and optimal patient care systems;
- Work in interprofessional teams to enhance patient safety and improve patient care quality;
- Participate in identifying system errors and implementing potential systems solutions.
-
Medical knowledge
Residents must demonstrate knowledge of established and evolving biomedical, clinical, epidemiological and social behavioral sciences, as well as the application of this knowledge to patient care. Residents must demonstrate competence in their knowledge of the basic and clinical sciences specific to ophthalmology. -
Practice-based learning and improvement
Residents must demonstrate the ability to investigate and evaluate their care of patients, to appraise and assimilate scientific evidence, and to continuously improve patient care based on constant self-evaluation and life-long learning.
Residents are expected to develop skills and habits to be able to meet the following goals:- Identify strengths, deficiencies, and limits in knowledge and expertise;
- Set learning and improvement goals;
- Identify and perform appropriate learning activities;
- Systematically analyze practice using quality improvement methods, and implement changes with the goal of practice improvement;
- Incorporate formative evaluation feedback into daily practice;
- Locate, appraise, and assimilate evidence from scientific studies related to their patients’ health problems;
- Use information technology to optimize learning;
- Participate in the education of patients, families, students, residents and other health professionals.
-
Interpersonal and Communication Skills
Residents must demonstrate interpersonal and communication skills that result in the effective exchange of information and collaboration with patients, their families,
and health professionals. Residents are expected to:- Communicate effectively with patients, families, and the public, as appropriate, across a broad range of socioeconomic and cultural backgrounds;
- Communicate effectively with physicians, other health professionals, and health related agencies;
- Work effectively as a member or leader of a health care team or other professional group;
- Act in a consultative role to other physicians and health professionals;
- Maintain comprehensive, timely, and legible medical records.
-
Duties and responsibilities of the PGY-1 integrated first year
At MedStar Washington Hospital Center, we have chosen to integrate the PGY-1 year into ophthalmology training to create a comprehensive four-year residency program.
In this integrated program, residents will have the opportunity to rotate through ophthalmology during their intern year for a total of three months.
The rest of the time will be divided between Internal Medicine and General Surgery to create a truly transitional year experience. There will be four weeks of vacation integrated throughout the year.
-
PGY 2
Second-year residents rotate through retina, glaucoma, and general clinics. The second-year residents are introduced to the operating room early in the year, first observing and then assisting in surgery.
Residents obtain advice from the attendings for any clinical finding or therapy of which they are unsure, and patients examined by residents during clinic hours are directly supervised by attending physicians.
Practice surgery utilizing both skin and microsurgical techniques is performed throughout the year and is emphasized at several wet labs during the year.
Residents also participate in a low vision clinic at MedStar Washington Hospital Center, affording the opportunity to learn management principles pertinent to this unique patient group. They are introduced to ophthalmic community service through attendance at the monthly Bread for the City clinics.
-
PGY 3
Third-year residents undergo a program that consists of rotations in comprehensive ophthalmology, pediatrics, cornea, neuro-ophthalmology, consults, ophthalmic pathology, refractive surgery, private practice, and research.
At the end of the third year, the residents have augmented and solidified their diagnostic expertise, participated in a mentored basic or clinical research project (presented on Residents Day), developed facility with the operating microscope and surgical techniques, have attended more than 20 surgical morbidity conferences during which they have learned how to manage all types of operative and post-operative complications, and performed 10 to 20 cataract and 20 to 30 miscellaneous muscle or adnexal operations. In addition, they have attended an ocular trauma course and a cataract course.
-
PGY 4
Fourth-year residents rotate through MedStar Washington Hospital Center and the VA and Fairfax Eye Clinics, and have ample opportunity for surgical experience in a wide variety of cases, directly supervised by a diverse and fully qualified attending staff.
The final-year resident schedule is designed to offer the longest possible opportunity for pre-op, operative, and post-operative management of a demographically diverse clinic population.
At the conclusion of the third year, residents have performed more than 2,000 ocular surgical procedures as primary surgeon and have participated in more than 3,000 surgeries as both primary surgeon and first assistant.
-
Surgical curriculum
The Eye Surgical Training Program is an integral part of the MedStar Georgetown University Hospital/MedStar Washington Hospital Center ophthalmology residency. Basic science instruction, intensive general eye clinic experience, comprehensive and sub-specialty rotations on- and off-campus, in-hospital consultation service, faculty and visiting lectures, rounds, and workshops are fully integrated into the curriculum. It culminates in a senior year in which the residents assume charge of their own clinic practices, under direct attending supervision, during which time they evaluate and medically and surgically manage their own patients. These patients shall at all times be treated respectfully, compassionately, and competently by all residents and staff. The MGUH/MWHC residency has developed a graded program of observation, instruction, and experience, with increasing levels of responsibility in order to train high quality clinical ophthalmologists. Resident surgical experience is obtained at the following affiliated sites: MedStar Washington Hospital Center (MWHC); MedStar Georgetown University Hospital (MGUH); MedStar St. Mary’s Hospital (MSMH); Department of Veteran Affairs Medical Center (VA); Childrens National Medical Center (CNMC), and Fairfax Hospital (FFX). Surgical training in ophthalmology is described below.
Wet lab experiences are scheduled throughout the academic year. This surgical skills development resource provides progressive instruction, under direct faculty supervision, on the basics of suturing and performance of intraocular surgical procedures. Additionally, a Simulator curriculum is designed to assess residents’ progress through all aspects of ocular surgery for the entire residency. ALL resident surgical procedures are done under the direct supervision of an attending ophthalmologist.PGY2
In August and September of each year the Eye Chief Residents arrange a series of faculty lectures to introduce the PGY2 residents to ophthalmic surgery. These lectures are a minimum of four hours, and include the following:
- Technical aspects - sutures, needles, instruments, microscopes, etc.
- Basic surgical techniques - skin, conjunctival, and corneo-scleral incisions, suturing and tying, wound healing, ophthalmic anesthesia, surgical physiology and pharmacology, etc.
- Common surgical procedures - cataract/IOL, glaucoma, YAG and argon/dye laser, scleral buckle, vitrectomy, etc.
Before the fall of each academic year, the Eye Chief Residents have arranged operating room in-services with the Eye OR Head Nurse at all sites to familiarize all residents with the following procedures and equipment:
- Location of all OR facilities - PACU, Eye OR's, Perioperative Care, lockers, lounges, etc.
- Eye OR procedures - scrubbing, prepping, gowning/gloving, hospital chart requirements, dictation, OR supplies, etc.
- Set up of the following OR equipment:
a. Phaco, Vitrectomy, and I/A modules
b. Operating Room and Clinic Microscopes
c. Video equipment and monitors (OR’s and Clinic)
d. Eye stretchers, chairs, basic sterile instrument set-up.
Eye Residents must obtain 2.0 to 3.5X loupes by September 1 of their first year.
After observing in surgery in the afternoons during the Basic Science course, residents begin, where appropriate, to first assist in the ORs. It is the responsibility of the eye chief residents to rotate junior residents through a wide-ranging experience as first assistants.
Residents begin their on-line surgical log in August, which all residents maintain for inspection by the Program Director or his/her designee at any time.
Residents are assisted, through September, by a senior resident or attending physician on all minor trauma and minor surgery. Residents become proficient in sub-specialty, non-refractive laser procedures.Residents become proficient in keratometry, optical and ultrasonic pachymetry and biometry, and are familiar with the basics of ophthalmic microsurgery. They prepare themselves for their rotations at the VA, MGUH, MWHC, and WRB by:
- Becoming proficient at hand and instrument tying and suturing appropriate practice materials with their loupes
- Practicing microsurgical incision and 22 micron tying on cadaver and/or fresh animal eyes with a surgical microscope, and
- Using a surgical simulation tool, if available.
At the end of PGY2, residents have a complete understanding of the technical aspects of ophthalmic surgery, including major equipment, disposables, basic procedures, operating room decorum, etc.
PGY3
PGY3 residents begin to develop an understanding and appreciation of the ethical, psychological, and practical aspects of surgical therapeutics.
- Residents study appropriate general and pediatric surgical atlases, texts and articles, and, if possible, observe several surgical cases at CNMC prior to starting their rotation there.
- Residents maintain careful awareness of general and pediatric cases done and posted by the preceding resident at VA, FFX and CNMC, who cooperates to ensure that an adequate number of cases is scheduled for the limited operating time available to the in-coming resident.
Residents arrange for at least two sessions of practice surgery on cadaver eyes, for the express purpose of further developing facility in suturing and tying under the operating microscope with 22 micron suture. Additionally, experience in incisional refractive surgery is obtained through practice on cadaver or fresh animal eyes. At least one session must be supervised by an attending physician.
Residents post and perform their own cases at MWHC when they begin to take Senior call.
PGY3 residents are responsible for preparing and presenting all of the surgery-related material in the Basic Science Course of the American Academy of Ophthalmology.By the end of the second year, residents are emotionally and intellectually prepared to administer a busy clinic and surgical practice. They have clear ideas of surgical goals and limitations. They are able to present a surgical candidate for attending approval clearly, concisely, completely, and efficiently. They have in-depth knowledge of instruments, sutures, needles, techniques, surgical anatomy, physiology, and pathology, and are prepared to begin the process of developing the art and science of surgical decision making. They have performed 15-20 cataract surgeries as primary surgeon while on rotation at MedStar Washington Hospital, VA and FFX, have performed muscle and other pediatric surgical procedures as primary surgeon at CNMC and MGUH, and have performed several anterior segment surgeries as primary surgeon at MedStar Georgetown and MedStar Washington Hospital.
PGY4
Senior eye residents, under attending supervision at MedStar Washington Hospital, MedStar St. Mary's Hosptial, VA, and FFX integrate complete eye care to their clinic patients. They see that all medical and administrative approvals, pre-operative general medical and ophthalmologic evaluations, signed informed consents, post-operative dispositions, equipment availability, patient notification and instruction, and other pre-operative requirements are complete and available to the attending surgeon no less than 24 hours prior to the scheduled surgery. All surgical cases are reviewed and approved by attending ophthalmologists prior to posting.
Residents perform all surgeries under the direct supervision of an attending surgeon.
Residents have sub-specialty clinic and senior call responsibilities. Sub-specialty assignment for consultation, evaluation, and surgery is rotated among the senior eye residents.
The two chief residents monitor the caseloads of the various operating residents to ensure a reasonably equitable distribution of common surgical procedures and a more strictly equitable distribution of complicated and rarer cases, such as penetrating keratoplasties, unusual oculoplastics, complex cataract etc.
Senior residents are expected to show good surgical judgment in selection of patients for phacoemulsification.
Residents are responsible individually or collectively to prepare and present their cases at the monthly M&B (Morbidity and Blindness) Rounds. The purpose of M&B Rounds is, in addition to a review of all clinic cases done by the residents, an essential discipline for self-evaluation and self-criticism.
Residents have adjunct surgical teaching responsibilities. They help prepare their junior residents as indicated in this syllabus. They practice as positive examples with the highest medical standards, with unwavering concern to put and keep the patient's welfare foremost.
By the end of the eye residency, residents have acquired the ability to appropriately evaluate and perform a wide range of ophthalmic surgical procedures. There is a harmonious synthesis of all of the elements of pre-, intra-, and post-operative care. Residents clearly understand that ophthalmic surgery is an evolving and heterogeneous field that will require a continuous process of discriminating learning for the rest of their careers. -
Schedule and call
At MWHC residents share coverage for emergency night call during the PGY2 year. PGY3 residents cover 20 nights per resident per year. Third-year residents are on stand-by call. An ophthalmology resident is on duty at MWHC to handle calls until 6:00 p.m. weeknights; thereafter, calls are taken from home by pager. Depending on the service, severity and volume of cases, calls at all facilities are managed via pager. Call duties at the other rotations, if assigned, vary by institution and by year.
All resident schedules are drawn up by the chief residents and are approved by the program director.
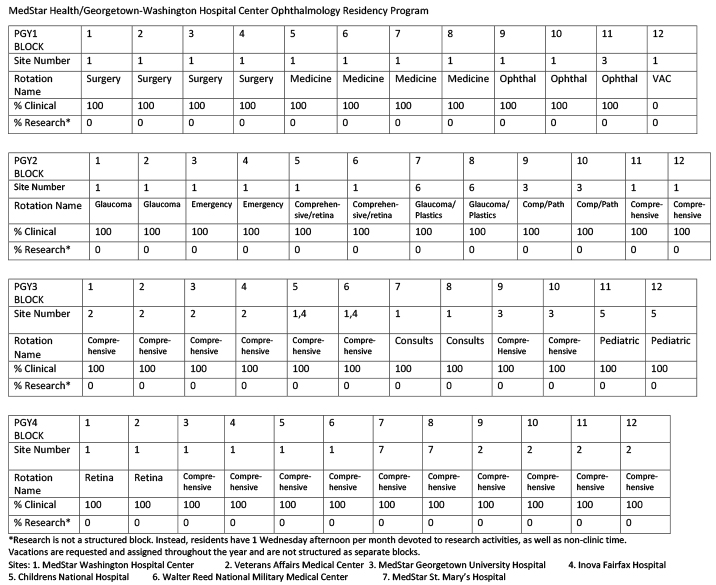
Sample Rotation Schedule -
Didactics and conferences
Regularly scheduled didactics are held nearly every Wednesday afternoon, for a minimum of 3 hours per week. These lecture sessions cover a multitude of topics in the basic and clinical sciences in ophthalmology. Topics include: cataract surgery, contact lenses, cornea and external disease, eyelid abnormalities, glaucoma, neuro-ophthalmology, ocular trauma, optics and refraction, orbital disease and ophthalmic plastic surgery, pathology, pediatric ophthalmology and strabismus, systemic disease consults, uveitis, visual rehabilitation, refractive surgery, and vitreo-retinal diseases. In addition, the following topics are also discussed: advocacy, ethics, practice management, and socio-economics.
In addition to the weekly didactic sessions, the residents participate in many other conferences. The annual Lecture Series includes a neuro-ophthalmology invited lecture, an Alumni and Resident Research symposium, a retina symposium, a low vision symposium, and a billing and coding seminar. Most of these sessions include resident case presentations and discussions and feature prominent speakers from around the country as well as members of the program’s faculty.
The monthly Morbidity and Blindness Rounds consist of faculty discussion of cases presented by the residents of surgical complications encountered in their own and attending surgeons’ cases. Monthly retina conferences, ocular motility, neuro-ophthalmology, cornea and oculoplastics rounds are also conducted, at which interesting cases are presented by the residents for discussion. At the quarterly Department meetings, an innovative “point-counterpoint” format allows residents to research and present current thinking on a controversial ophthalmology topic. Visiting Professors are scheduled at MedStar Georgetown University Hospital, including an hour of case presentations by the residents, and discussion of the cases as well as lectures by the Visiting Professor.
The retina service holds monthly intravenous fluorescein rounds. This is a case-based series which covers basic and advanced diagnostic interpretations of retinal fluorescein and indocyanine green (ICG) images.
In addition to these scheduled conferences in which all of the residents participate, there are formal teaching case presentations at each rotation site, coordinated by the local site director. -
During the course of their training, the residents are actively involved in the care of patients with a wide variety of ophthalmic diseases. The program seeks to foster increasing independence in the evaluation, diagnosis, and treatment of patients as the four years progress, as well as continuity of care. Case loads are gradually increased during the PGY2 year as the resident acquires increased clinical skills and increased clinical confidence. As the residents progress through the program, their skills and knowledge continue to improve, allowing them to see more patients and develop increasing independence, so that they are able to practice independently upon completion of the program. However, this independence is accompanied by supervision throughout the their years of training. For example, at MWHC, every clinic patient is examined by an attending physician after the evaluation by the resident, allowing for immediate feedback on the aspects of the resident’s examination. At MGUH, the patients are generally the private patients of the faculty, but each is examined by the resident before the faculty member’s evaluation. Patients are discussed at the end of the day, and pertinent findings on the patient’s examination are discussed. At each rotation site, attendings are always present when residents are examining patients during normal working hours, allowing for 100% supervision.
Specific duties and responsibilities at each level of training
-
The PGY1 Integrated First Year
At MedStar Washington Hospital Center, we have chosen to integrate the PGY1 year into ophthalmology training to create a comprehensive 4-year residency program. In this integrated program, residents have the opportunity to rotate through ophthalmology during their intern year for a total of 3 months. The rest of the time is divided between Internal Medicine and General Surgery to create a truly transitional year experience. There are 4 weeks of vacation integrated throughout the year.
During their time on the Internal Medicine service, ophthalmology residents have a chance to rotate on the internal medicine wards, treating a variety of diagnoses and honing the physical exam and diagnostic skills attained during their medical school clerkships.
While on the General Surgery service, ophthalmology residents have the opportunity to rotate on the surgical wards, treating both preoperative and postoperative patients. This reinforces important pre and postoperative management which will aid in their future surgical careers.
Finally, during the ophthalmology months, residents learn important slit lamp and refraction skills. They also get the opportunity to take part in the inpatient consultation service and coordinate eyecare throughout the hospital with a variety of different services. The ocular pathology is unparalleled at our program, and the PGY1 residents take full advantage of this to create a strong foundation in ophthalmology.
PGY1 Rotation Schedule
4 months Internal Medicine
4 months General Surgery
3 months Ophthalmology clinic/consultation service
1 month vacation spread through IM, Surgery and Ophthalmology -
PGY2 residents rotate through retina, glaucoma, and general clinics at MedStar Washington Hospital Center, MedStar Georgetown University Hospital, and WRB, as well as assist in surgery at these locations. Caseloads are adjusted to the expertise and experience of the first year residents.
A basic science course at the beginning of the PGY2 year serves as an introduction to ophthalmology. When not in class, residents learn the ophthalmologic examination by doing histories and eye examinations. They also begin to learn the fundamental procedures of refraction, tonometry, retinoscopy, biomicroscopy, gonioscopy, indirect ophthalmoscopy, visual field interpretation and the use of the potential acuity meter.
Residents gain experience in retinal disease, uveitis, diagnostics and therapeutics, make fundus drawings of the detachment cases, and assist in surgery on many of the cases they have drawn. The residents also assist on vitrectomies. They learn to interpret fluorescein angiograms and OCT’s both in the daily clinic and in the monthly fluorescein conferences. The residents, under direct supervision, perform retinal laser therapy and intravitreal injections.
The weekly Glaucoma Review Board at MedStar Washington Hospital features five to seven problem cases completely worked up and presented to the subspecialty attendings by the residents assigned to the glaucoma service. In addition, the glaucoma subspecialty clinic at MedStar Georgetown allows the resident the opportunity to participate in the diagnosis and management of a large number of private attending glaucoma patients. Gonioscopy instruction is carried out in a one-on-one manner. The residents, under direct supervision, perform laser trabeculoplasties and iridotomies.
The balance of the PGY2 year is devoted to the diagnosis and therapy of patients in the general eye clinics at MedStar Washington Hospital, MedStar Georgetown and WRB, including emergency and consultative cases. Residents are introduced to the operating room early in the year, first observing, and then assisting in surgery. Residents obtain advice from the attendings for any clinical finding or therapy of which they are unsure, and patients examined by residents during clinic hours are directly supervised by attending physicians. Practice surgery utilizing both skin and microsurgical techniques is performed throughout the year and is emphasized at several wet labs during the year.
Residents participate in a low vision clinic at MedStar Washington Hospital, affording the opportunity to learn management principles pertinent to this unique patient group. They are introduced to ophthalmic community service through attendance at glaucoma screenings and lectures to low vision support groups.
At the conclusion of the PGY2 year, residents have developed a functional facility in all of the standard diagnostic techniques, as well as a solid grounding in the diagnosis and management of a variety of eye diseases. Case histories, clinical examinations and minor incisional and laser surgical procedures are performed with competence. Extensive experience as first assistant in a wide variety of intra- and extra-ocular cases gives them a solid foundation in operating room comportment and procedures. They have presented a research poster during the annual Residents’ Day. -
PGY 3
PGY3 residents undergo a program which consists of rotations in comprehensive ophthalmology, pediatrics, cornea, neuro-ophthalmology, consults, ophthalmic pathology, refractive surgery, private practice and research.
The Pediatric rotation takes place at CNMC and MedStar Georgetown University Hospital. Evaluation and management of common and unusual pediatric ocular disease occurs in the setting of a busy pediatric referral center and a busy private practice with fellowship-trained pediatric ophthalmologists. Residents evaluate and operate on their own and private strabismus patients, and participate in the management of other acute and chronic pediatric eye disease as well as adult strabismus.
The Consult Service occurs at MedStar Washington Hospital Center, MedStar Georgetown and the VA. For this rotation, residents are responsible for the management of all patients who have had a formal consultation requested of ophthalmology by other specialties. This experience gives the residents an outstanding opportunity to learn about the interactions of ophthalmology with a multitude of systemic diseases.
At MGUH, residents learn to grossly examine enucleated globes and other ocular tissues, prepare them for histopathologic examination and conduct that examination under the supervision of a fellowship-trained staff ophthalmic pathologist. A strong foundation in ophthalmic pathology is also provided for the residents by slide reviews and by attendance at the several special ophthalmic pathology didactic sessions. Residents become proficient in the gross and microscopic examination of eyes and other tissue specimens sent for evaluation to MedStar Georgetown as well as in the correlation of microscopic findings with clinical data, which significantly enhances their understanding of ophthalmic diseases. The residents may participate in research projects analyzing some aspects of these case materials. Training in the use and fitting of contact lenses occurs under the supervision of a certified OD.
In addition, while at MedStar Georgetown, residents participate in the clinical and surgical care of patients with a variety of anterior segment and cornea problems. They learn to diagnose and manage a variety of common and unusual cornea and anterior segment diseases. For those patients needing surgery, the residents are involved in their preoperative, intraoperative, and postoperative care, either as primary surgeon or as first assistant. Direct faculty supervision of all patients occurs. Residents also participate in a tertiary care neuro-ophthalmology clinic, performing the initial examination and suggesting diagnostic and therapeutic approaches. This experience is an excellent adjunct to the neuro-ophthalmology experience at MedStar Washington Hospital that occurs throughout all three years of training.
Microsurgical suturing is practiced in the MedStar Washington Hospital Eye Center Wet Lab and in the eye operating room at MedStar Washington Hospital. By the time the residents are ready to perform their first cataract operations, they have assisted in over 100 private cases, performed segments or the entirety of some cases, done enucleations and eyelid procedures under supervision, and have become proficient in the use of the operating microscope and microsurgical techniques in practice surgery sessions. Careful pre-operative and post-operative attention to detail is stressed, and above all, the importance of visual rehabilitation. Residents are made aware that the program has enjoyed a solid reputation based on many years of providing ophthalmologic care to the community, and that each resident is a vital link in this unbroken chain. Experience as primary surgeon commences in earnest in the PGY3 year, with resident cataract surgical cases as primary surgeon beginning at the VA, MedStar Washington Hospital and FFX. Resident surgical training is outlined further in the Surgical Curriculum.
At the end of the PGY3 year, the residents have augmented and solidified their diagnostic expertise, participated in a mentored basic or clinical research project (presented on Residents' Day), developed facility with the operating microscope and surgical techniques, have attended more than 20 surgical morbidity conferences during which they have learned how to manage all types of operative and post-operative complications, performed ten to twenty cataract and twenty to thirty miscellaneous muscle or adnexal operations. In addition, they have attended an ocular trauma course and a cataract course. -
PGY4 residents rotate through MedStar Washington Hospital Center, MedStar St. Mary's Hospital Center, VA and FFX Eye Clinics, and have ample opportunity for surgical experience in a wide variety of cases, directly supervised by a diverse and fully qualified attending staff. It is highly desirable, and the final year resident schedule is designed, to offer the longest possible opportunity for pre-op, operative, and post-operative management of a demographically diverse clinic population. Senior residents also have the option to participate in an international mission trip, usually for one week, during which time they receive first-hand experience with the rigors and difficulties involved with obtaining adequate medical and surgical treatment in Third World countries.
During the PGY4 year, residents are in the operating room one to two days per week, assisting and performing surgery on their own cases, always under direct attending supervision. In the clinics, the day is spent seeing pre-operative and post-operative cases as well as a large variety of cases from the general clinic and subspecialty clinics. Operative and post-operative complications are reviewed at a monthly surgical morbidity conference. In addition, residents participate in the cornea clinic, the oculoplastics clinic, retina clinic, and the glaucoma review board, and perform laser surgery on selected cases approved by a glaucoma, refractive or retina attending. It is expected that the PGY4 rotations provide clinical and surgical opportunities for education, diversity of patients and attending physicians and practice environment, to better prepare residents for their subsequent fellowships and careers.
Residents have an intensive retina rotation at MedStar Washington Hospital. During these 2 months, they actively participate in the diagnosis and management of a variety of complex retinal diseases. They work with experienced subspecialty attendings, retina fellows, and junior residents, and perform both laser and intraocular retinal surgeries as primary surgeon.
At the conclusion of the PGY4 year, residents have performed more than 2000 ocular surgical procedures as primary surgeon and have participated in more than 3000 surgeries as both primary surgeon and first assistant. Throughout the residency, each resident must enter his or her surgical cases into the ACGME Case Log System, including those as primary surgeon as well as first assistant. Case Logs are monitored weekly by the Program Director.
PGY4 residents develop sound judgment and technical expertise in the management of surgical and medical cases, and are fully prepared to practice competently and independently upon completion of their training.
Rotations
Research
Scholarly activity is encouraged in the program in a variety of ways. Residents are taught the basic principles of clinical research during their weekly didactics. They learn how to conduct research and utilize basic principles of data analysis. They learn how to obtain approval for projects through the MedStar Washington Hospital Center or MedStar Georgetown University Hospital Institutional Review Board. PGY2 residents present posters of their preliminary research ideas at the Residents Day in June. There is protected time for residents to continue to refine their projects, conduct studies, and meet with faculty mentors regarding their projects. Each PGY3 and PGY4 resident does a presentation of their research project at Residents Day. When funding is needed for research, the Department is able to provide the financial resources needed for the resident’s project. When statistical analysis is needed, the Department of Biostatistics at Georgetown University is available to work with the resident in their data analysis. Basic science research is also available to residents at MGUH.
The program further encourages resident research by sponsoring their attendance at scientific meetings where their studies are presented. This encourages residents to produce high quality studies for presentation at national ophthalmology meetings and publication in peer-reviewed journals.
Additionally, The Ocular Innovation Award is given annually to the ophthalmology residency program to support resident research as well as to the resident who has been judged to have produced during the year the best original concept, operation, instrument or invention in ophthalmology. This award was established in 2013 by Dr. John Karickhoff, a former Attending Faculty Member of the MedStar Georgetown University Hospital/Washington Hospital Center ophthalmology residency program.
By the end of a resident’s course of study in ophthalmology, they have presented research at an average of 12-15 major local, regional and national meetings and served as presenter or lecturer for numerous sessions/events, including the monthly Low Vision Support Group at MWHC and the bi-monthly department medical staff meetings.
WELLNESS in the MedStar Georgetown University Hospital/Washington Hospital Center Ophthalmology Residency Program
Through a collaboration with MedStar Health and the Washington National Eye Center, the Ophthalmology residents participate in a Wellness Curriculum during their training. The annual curriculum includes quarterly group lectures with decompression sessions, large group events (such as baseball games and bowling nights), physical fitness activities (including an annual 5K), an annual team-building retreat, and access to mental health resources within the MedStar hospital system. The residents enjoy social events during the year to celebrate milestones and holidays, including Thanksgiving dinner, post-OKAP’s happy hour, and graduation celebrations. Through resident feedback and involvement, the Ophthalmology Department's Wellness Curriculum provides multifaceted support for a balanced training experience during residency.
Underrepresented in Medicine Scholarship Program (URIM)
A scholarship program for medical students who are underrepresented in medicine has been implemented, This important program provides support to medical students to allow them to complete a one month visiting student rotation in our Department. Often these students cannot afford the costs of such an experience, depriving them of important opportunities.
Each selected student receives a scholarship, with the cost split between Washington National Eye Center and MedStar Health Office of Graduate Medical Education.
For the 2025-26 rotations, we are continuing to sponsor students to receive these scholarships.
Training locations
Washington National Eye Center, Inc. at MedStar
Washington Hospital Center,
110 Irving Street, NW, Suite 1A-19,
Washington, D.,C 20010
MedStar Georgetown University Hospital
3800 Reservoir Road, NW,
Pasquerilla Healthcare Center, Lower Level,
Washington, D.C., 20007
Washington, D.C., Veterans Affairs Medical Center
50 Irving Street, NW,
Ophthalmology Section,
Washington, D.C., 20422
INOVA Fairfax Hospital
3299 Woodburn Road, #150,
Annandale, VA 22003
Walter Reed National Military Medical Center
8901 Rockville Pike,
Bethesda, MD 20889
Children's National Medical Center
111 Michigan Avenue, NW,
Washington, DC 20010
MedStar St. Mary's Hospital
2550 Point Lookout Road,
Leonardtown, MD 20650
Application information
Interested in applying?
Contact us
Penelope Helfgott
Administrative Program Director
202-877-5329
penelope.a.helfgott@medstar.net