The MedStar Health—Georgetown University Hospital Residency Program in Neurological Surgery
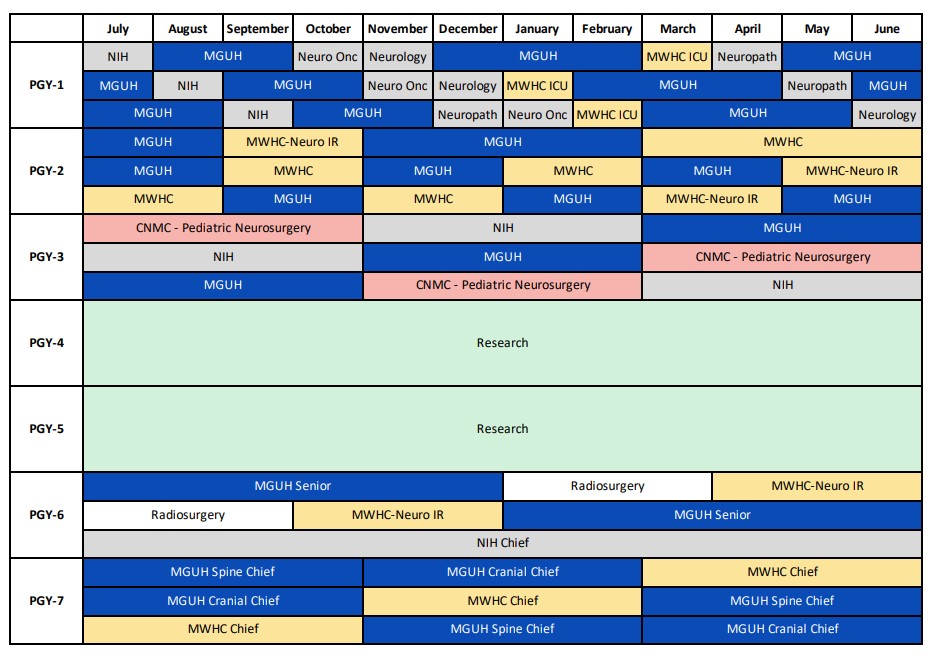
MedStar Georgetown Neurosurgery residency program, in partnership with the National Institute of Health, offers a seven-year training program in Neurological Surgery. The two programs collectively accept three residents each year (two at Georgetown, and one at the NIH) all of whom train together in one combined residency program and complete the exact same rotations with the exception of the PGY-6 year, during which the NIH resident serves as the Chief Resident at NIH. Our residents rotate through four affiliated institutions including MedStar Georgetown University Hospital (MGUH), MedStar Washington Hospital Center (MWHC), the National Institute of Health (NIH), and Children’s National Hospital (CNH), and they and are involved in more than 3000 neurosurgical procedures at these hospitals each year. Throughout their training, they are exposed to the full spectrum of neurosurgical subspecialties including:
- Skull Base Surgery
- Neuro-Oncology
- Cerebrovascular Surgery
- Endovascular/Neurointerventional
- Spine Surgery
- Pediatric Neurosurgery
- Functional Neurosurgery
- Trauma and Neurocritical Care
- Peripheral Nerve
To learn more about the experience of this residency, read this letter from the Chairman and Program Director. Open Now.
Why train here
MedStar Georgetown University Hospital is the central site of the program, and our residents rotate through the hospital at all levels of training. Special features of this hospital relevant to their training include multi-disciplinary teams for neuro-vascular (with neuro-radiology), spine (with orthopedics), and skull base surgery (with otolaryngology).
The movement disorder program is also run jointly with the department of neurology, and is always busy with deep-brain stimulation procedures. MedStar Georgetown has two CyberKnife® radiation delivery systems, and our trainees are intimately involved with radiosurgical cases during their rotations.
Contact us
If you have any questions or would like further information about the Neurosurgery Residency Program or medical student rotations, please contact the residency program and medical student coordinator, Olujie Ifegwu, at Olujie.v.ifegwu@gunet.georgetown.edu.