Featured News
-
June 08, 2026
SILVER SPRING, Md. — MedStar Health marked CPR & AED Awareness Week with its third annual training event held at Montgomery Blair High School. Nearly 100 attendees learned bystander CPR and ...
Browse news by hospital and team
For reporters
Share this
All News
-
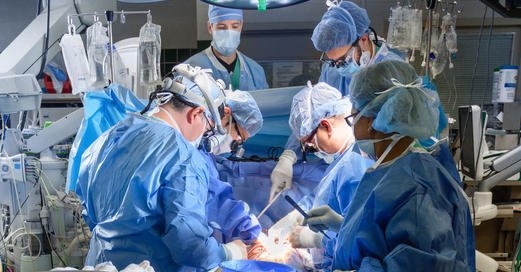 July 20, 2020
July 20, 2020MedStar Heart & Vascular Institute Performs Record Number of Heart Transplantation Washington, D.C. – While some hospitals across the country paused or reduced organ transplants, MedStar Hea...
-
 July 17, 2020
July 17, 2020Washington, D.C.,– While government stay-at-home orders helped to slow the spread of the coronavirus, it had some unintended consequences: more people were getting burned in the kitchen. The Burn Cent...
-
 July 16, 2020The Federal Communications Commission (FCC) has awarded $976,679 to MedStar Health to provide additional support for the exponential growth of the system’s telehealth offerings in response to COVID-19. As of early July, MedStar Health had delivered more than 275,000 telehealth sessions during the pandemic.
July 16, 2020The Federal Communications Commission (FCC) has awarded $976,679 to MedStar Health to provide additional support for the exponential growth of the system’s telehealth offerings in response to COVID-19. As of early July, MedStar Health had delivered more than 275,000 telehealth sessions during the pandemic. -
July 16, 2020During the peak of the spring 2020 COVID-19 outbreak, MedStar Health conducted more than 4,500 telehealth encounters each weekday to ensure safe and efficient care for our patients, providers, and communities. By May 1, the system had reached the significant milestone of more than 100,000 telehealth sessions delivered in total during the pandemic.
-
July 06, 2020
Study data may explain why COVID-19 patients with clinically recognized predisposing factors like obesity, diabetes, liver, kidney and heart disease have more severe disease WASHINGTON –A study ...
-
July 01, 2020
New safety protocol allowed all transplants and related services to continue uninterrupted. WASHINGTON, D.C. — During the height of the COVID-19 pandemic, MedStar Georgetown Transplant Institute...
- 1
- 2
- 3
- 4
- 5
- 6
- 7
- 8
- 9
- 10
- 11
- 12
- 13
- 14
- 15
- 16
- 17
- 18
- 19
- 20
- 21
- 22
- 23
- 24
- 25
- 26
- 27
- 28
- 29
- 30
- 31
- 32
- 33
- 34
- 35
- 36
- 37
- 38
- 39
- 40
- 41
- 42
- 43
- 44
- 45
- 46
- 47
- 48
- 49
- 50
- 51
- 52
- 53
- 54
- 55
- 56
- 57
- 58
- 59
- 60
- 61
- 62
- 63
- 64
- 65
- 66
- 67
- 68
- 69
- 70
- 71
- 72
- 73
- 74
- 75
- 76
- 77
- 78
- 79
- 80
- 81
- 82
- 83
- 84
- 85
- 86
- 87
- 88
- 89
- 90
- 91
- 92
- 93
- 94
- 95
- 96
- 97
- 98
- 99
- 100
- 101
- 102
- 103
- 104
- 105
- 106
- 107
- 108
- 109
- 110
- 111
- 112
- 113
- 114
- 115
- 116
- 117
- 118
- 119
- 120
- 121
- 122
- 123
- 124
- 125
- 126
- 127
- 128
- 129
- 130
- 131
- 132
- 133
- 134
- 135
- 136
- 137
- 138
- 139
- 140
- 141
- 142
- 143
- 144
- 145
- 146
- 147
- 148
- 149
- 150
- 151
- 152
- 153
- 154
- 155
- 156
- 157
- 158
- 159
- 160
- 161
- 162
- 163
- 164
- 165
- 166
- 167
- 168
- 169
- 170
- 171
- 172
- 173
- 174
- 175
- 176











