Featured News
-
April 07, 2026
Carrington designed the colorful pants himself to give back to frontline healthcare workers in both DC and his hometown of Baltimore. WASHINGTON — By the time the first boxes were opened, excite...
Browse news by hospital and team
For reporters
Share this
All News
-
 February 17, 2021
February 17, 2021Philanthropic Contribution will Fund Mobile Health Center Providing COVID-19 Vaccine to Underserved Communities Columbia, MD –The Verstandig Family Foundation - a philanthropic organization est...
-
February 09, 2021
MedStar St. Mary’s to offer increased access to prevention programs Leonardtown, MD – Thanks to funding from Maryland’s Health Services Cost Review Commission (HSCRC) Regional Partn...
-
 February 08, 2021
February 08, 2021Leapfrog Hospital Safety Grade announces fall 2020 recognitions Leonardtown, MD – MedStar St. Mary’s Hospital was awarded its fifth “A” grade in December 2020 from the Leapfro...
-
 February 01, 2021MedStar Health Becomes First in Region to Take COVID-19 Vaccines to the Community with Mobile Clinic
February 01, 2021MedStar Health Becomes First in Region to Take COVID-19 Vaccines to the Community with Mobile ClinicMobile Strategy Begins in Cherry Hill with 65 People Vaccinated Baltimore, MD – MedStar Health became the first healthcare provider in the region to administer COVID-19 vaccines in the com...
-
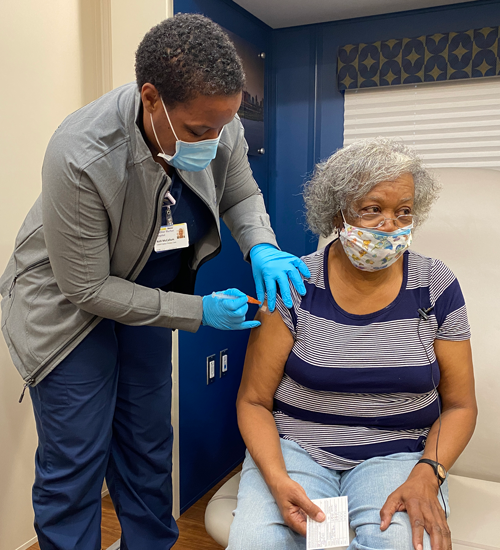 February 01, 2021
February 01, 2021Mobile Strategy Begins in Cherry Hill with 65 Vaccinated BALTIMORE—MedStar Health became the first healthcare provider in the region to administer COVID-19 vaccines in the community, when they vaccina...
-
January 26, 2021
Team will study technology used to access primary care surrounding COVID-19 and any related health disparities—and recommend actions to improve access for patients Columbia, MD—To bet...
- 1
- 2
- 3
- 4
- 5
- 6
- 7
- 8
- 9
- 10
- 11
- 12
- 13
- 14
- 15
- 16
- 17
- 18
- 19
- 20
- 21
- 22
- 23
- 24
- 25
- 26
- 27
- 28
- 29
- 30
- 31
- 32
- 33
- 34
- 35
- 36
- 37
- 38
- 39
- 40
- 41
- 42
- 43
- 44
- 45
- 46
- 47
- 48
- 49
- 50
- 51
- 52
- 53
- 54
- 55
- 56
- 57
- 58
- 59
- 60
- 61
- 62
- 63
- 64
- 65
- 66
- 67
- 68
- 69
- 70
- 71
- 72
- 73
- 74
- 75
- 76
- 77
- 78
- 79
- 80
- 81
- 82
- 83
- 84
- 85
- 86
- 87
- 88
- 89
- 90
- 91
- 92
- 93
- 94
- 95
- 96
- 97
- 98
- 99
- 100
- 101
- 102
- 103
- 104
- 105
- 106
- 107
- 108
- 109
- 110
- 111
- 112
- 113
- 114
- 115
- 116
- 117
- 118
- 119
- 120
- 121
- 122
- 123
- 124
- 125
- 126
- 127
- 128
- 129
- 130
- 131
- 132
- 133
- 134
- 135
- 136
- 137
- 138
- 139
- 140
- 141
- 142
- 143
- 144
- 145
- 146
- 147
- 148
- 149
- 150
- 151
- 152
- 153
- 154
- 155
- 156
- 157
- 158
- 159
- 160
- 161
- 162
- 163
- 164
- 165
- 166
- 167
- 168
- 169
- 170
- 171
- 172
- 173
- 174











