MedStar Health News | MedStar Health
Featured News
-
May 18, 2026
National Safe Sun Week highlights the importance of sunscreen use to prevent the most common form of cancer in the United States. COLUMBIA, Md. — MedStar Health wants everyone to lather up ...
Browse news by hospital and team
For reporters
Share this
All News
-
May 22, 2018Patients Experience Improved Quality of Life and Fewer Trips to the Emergency Department
-
 May 22, 2018Celebrates Launch of its Largest Innovative Sim Center Near MedStar Harbor Hospital
May 22, 2018Celebrates Launch of its Largest Innovative Sim Center Near MedStar Harbor Hospital -
May 17, 2018Learn about the treatment, recovery, and support process of two locals' experience with stroke and the care they received at MedStar St. Mary's Hospital.
-
 May 11, 2018
May 11, 2018With help from Maryland doctors, horse racing industry takes on concussions --> Kelly Ryan, DO, Sports Medicine Specialist and Member of the Maryland Horsemen's Health System staff, discusses concussi...
-
May 10, 2018
WASHINGTON, D.C., - MedStar National Rehabilitation Network Founder and Past President Edward A. Eckenhoff was honored with a special service at the Washington National Cathedral in early May. E...
-
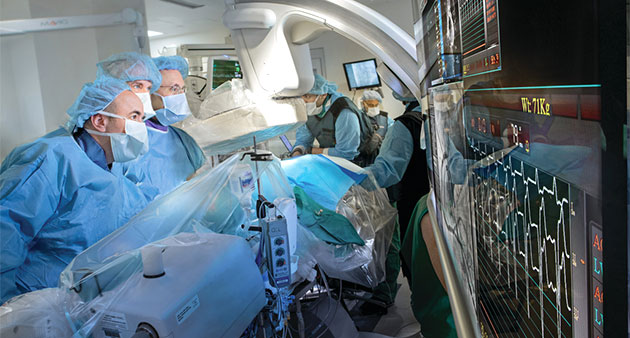 May 09, 2018Patients Undergoing Transcatheter Aortic Valve Replacement Showed No Deaths or Disabling Strokes within 30 days of Undergoing Less Invasive Procedure
May 09, 2018Patients Undergoing Transcatheter Aortic Valve Replacement Showed No Deaths or Disabling Strokes within 30 days of Undergoing Less Invasive Procedure
- 1
- 2
- 3
- 4
- 5
- 6
- 7
- 8
- 9
- 10
- 11
- 12
- 13
- 14
- 15
- 16
- 17
- 18
- 19
- 20
- 21
- 22
- 23
- 24
- 25
- 26
- 27
- 28
- 29
- 30
- 31
- 32
- 33
- 34
- 35
- 36
- 37
- 38
- 39
- 40
- 41
- 42
- 43
- 44
- 45
- 46
- 47
- 48
- 49
- 50
- 51
- 52
- 53
- 54
- 55
- 56
- 57
- 58
- 59
- 60
- 61
- 62
- 63
- 64
- 65
- 66
- 67
- 68
- 69
- 70
- 71
- 72
- 73
- 74
- 75
- 76
- 77
- 78
- 79
- 80
- 81
- 82
- 83
- 84
- 85
- 86
- 87
- 88
- 89
- 90
- 91
- 92
- 93
- 94
- 95
- 96
- 97
- 98
- 99
- 100
- 101
- 102
- 103
- 104
- 105
- 106
- 107
- 108
- 109
- 110
- 111
- 112
- 113
- 114
- 115
- 116
- 117
- 118
- 119
- 120
- 121
- 122
- 123
- 124
- 125
- 126
- 127
- 128
- 129
- 130
- 131
- 132
- 133
- 134
- 135
- 136
- 137
- 138
- 139
- 140
- 141
- 142
- 143
- 144
- 145
- 146
- 147
- 148
- 149
- 150
- 151
- 152
- 153
- 154
- 155
- 156
- 157
- 158
- 159
- 160
- 161
- 162
- 163
- 164
- 165
- 166
- 167
- 168
- 169
- 170
- 171
- 172
- 173
- 174
- 175










