Featured News
-
May 18, 2026
National Safe Sun Week highlights the importance of sunscreen use to prevent the most common form of cancer in the United States. COLUMBIA, Md. — MedStar Health wants everyone to lather up ...
Browse news by hospital and team
For reporters
Share this
All News
-
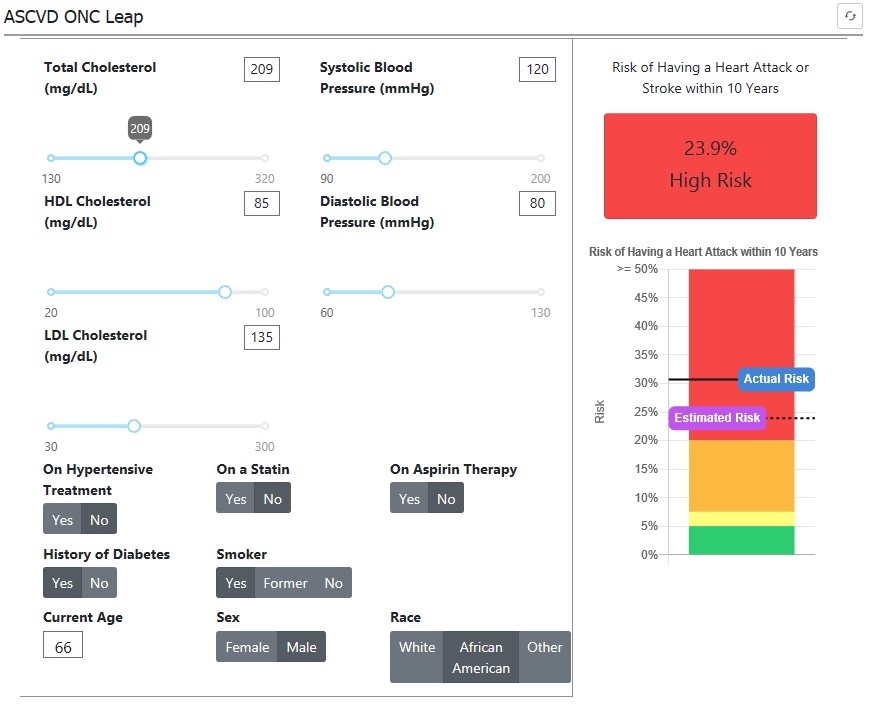 February 26, 2020MedStar Health is launching the first patient-facing, interactive heart risk calculator that will be integrated in its patients’ electronic health records (EHRs). An estimated 575 cardiologists and other doctors across the system will be able to more easily show patients their personal risk for heart disease, stroke, and other cardiovascular diseases over time using easy-to-read graphics. This assessment will help doctors recommend lifestyle choices to improve patients’ heart health, a topic that is top of mind each February during American Heart Month.
February 26, 2020MedStar Health is launching the first patient-facing, interactive heart risk calculator that will be integrated in its patients’ electronic health records (EHRs). An estimated 575 cardiologists and other doctors across the system will be able to more easily show patients their personal risk for heart disease, stroke, and other cardiovascular diseases over time using easy-to-read graphics. This assessment will help doctors recommend lifestyle choices to improve patients’ heart health, a topic that is top of mind each February during American Heart Month. -
February 10, 2020
Ryan Moran, Director of Community Health for MedStar Health’s three Baltimore hospitals, tells WJZ-TV that the unique fentanyl test kit program MedStar Health launched last September is off to a great...
-
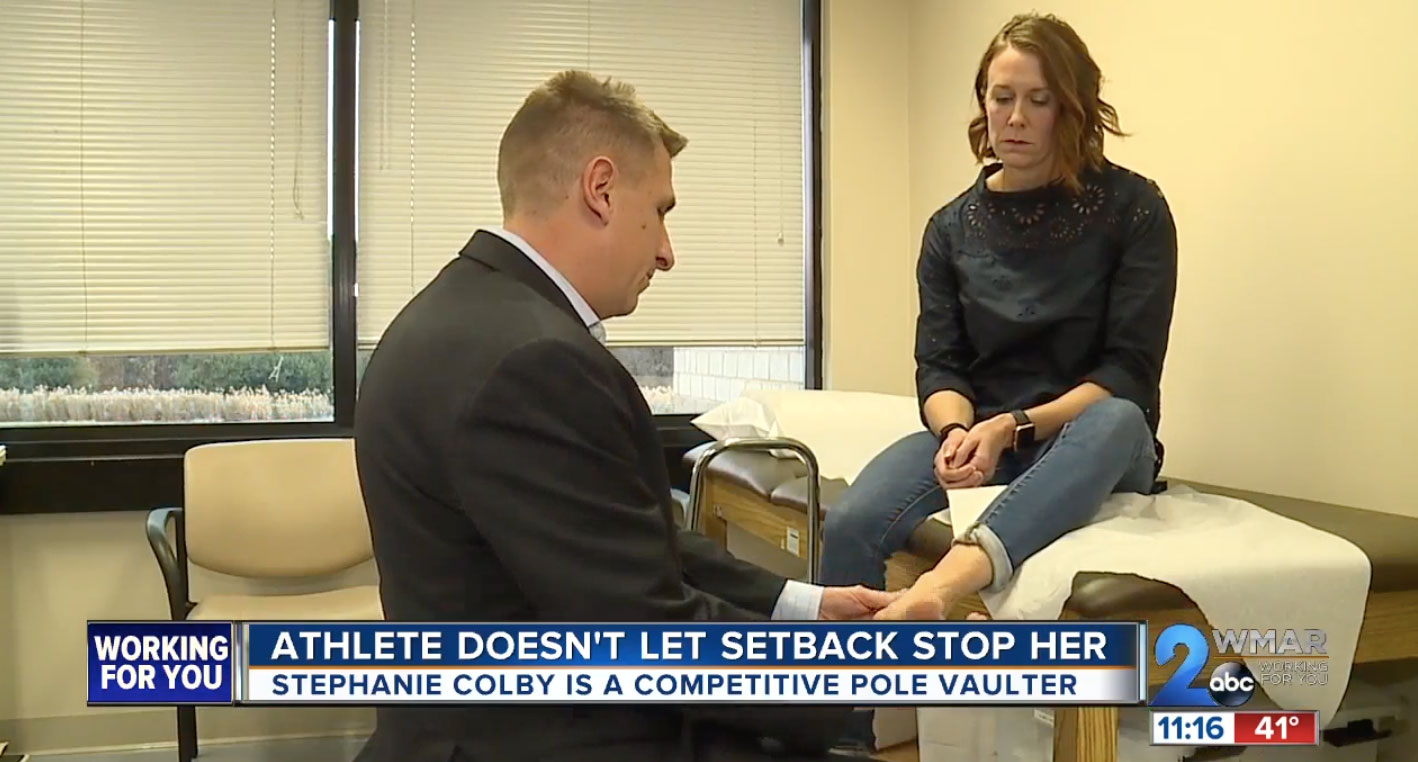 February 03, 2020
February 03, 2020Stephanie Coleman tore her Achilles’ tendon in the middle of a decathlon, but that didn’t stop her from finishing her last two events. And thanks to foot and ankle surgeon, Dr. Jake Wisbeck, it didn’t...
-
February 03, 2020
COLUMBIA, MD — MedStar Health is proud to announce it is a founding member and first health system to join the Cerner Learning Health NetworkSM, an innovative platform from Cerner Corporation (Na...
-
January 26, 2020An estimated 575 physicians across the MedStar Health system introduce tool allowing patients to see how lifestyle choices affect their risk for heart attack and stroke
-
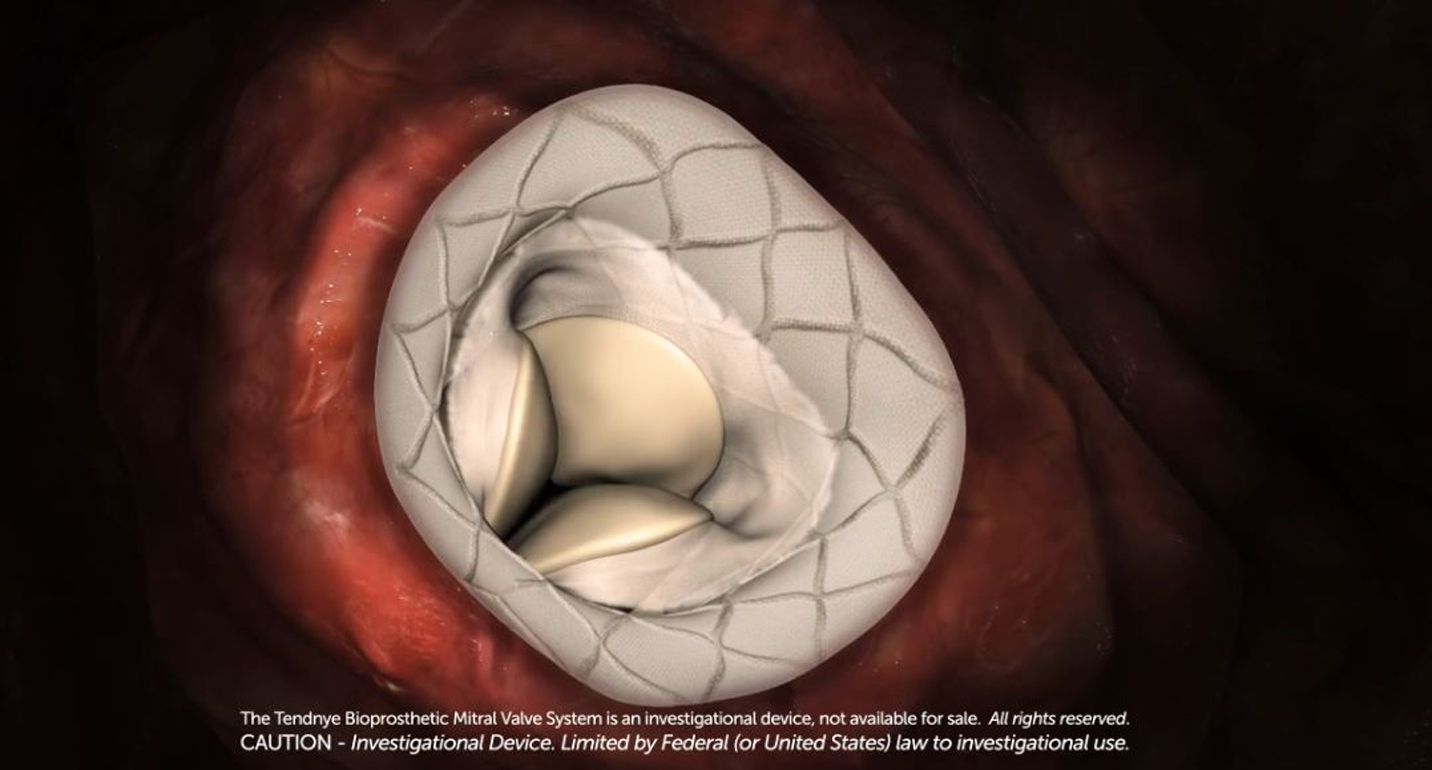 January 21, 2020MedStar Union Memorial Physician Implants Tendyne Valve Without Surgery
January 21, 2020MedStar Union Memorial Physician Implants Tendyne Valve Without Surgery
- 1
- 2
- 3
- 4
- 5
- 6
- 7
- 8
- 9
- 10
- 11
- 12
- 13
- 14
- 15
- 16
- 17
- 18
- 19
- 20
- 21
- 22
- 23
- 24
- 25
- 26
- 27
- 28
- 29
- 30
- 31
- 32
- 33
- 34
- 35
- 36
- 37
- 38
- 39
- 40
- 41
- 42
- 43
- 44
- 45
- 46
- 47
- 48
- 49
- 50
- 51
- 52
- 53
- 54
- 55
- 56
- 57
- 58
- 59
- 60
- 61
- 62
- 63
- 64
- 65
- 66
- 67
- 68
- 69
- 70
- 71
- 72
- 73
- 74
- 75
- 76
- 77
- 78
- 79
- 80
- 81
- 82
- 83
- 84
- 85
- 86
- 87
- 88
- 89
- 90
- 91
- 92
- 93
- 94
- 95
- 96
- 97
- 98
- 99
- 100
- 101
- 102
- 103
- 104
- 105
- 106
- 107
- 108
- 109
- 110
- 111
- 112
- 113
- 114
- 115
- 116
- 117
- 118
- 119
- 120
- 121
- 122
- 123
- 124
- 125
- 126
- 127
- 128
- 129
- 130
- 131
- 132
- 133
- 134
- 135
- 136
- 137
- 138
- 139
- 140
- 141
- 142
- 143
- 144
- 145
- 146
- 147
- 148
- 149
- 150
- 151
- 152
- 153
- 154
- 155
- 156
- 157
- 158
- 159
- 160
- 161
- 162
- 163
- 164
- 165
- 166
- 167
- 168
- 169
- 170
- 171
- 172
- 173
- 174
- 175











