Featured Blog
-
 May 15, 2026
May 15, 2026Lipids are the name for fats found in the blood and body tissues. Your body needs some lipids to build cells, but too much of certain types can be dangerous. The two main types we often talk about ar...
Browse blogs by hospital
Share this
All Blogs
-
 November 24, 2019
November 24, 2019By MedStar Health Research Institute
Georgetown-Howard Universities Center for Clinical and Translational Science (GHUCCTS) is now accepting applications for its KL2 Junior Faculty Scholars Program. Projects that are novel, inter- or mul...
-
 November 24, 2019
November 24, 2019By MedStar Health Research Institute
Recently published research evaluated nurse and patient care technician workflow to identify opportunities for providing education to patients during care. The study sought to examine the feasibility ...
-
 November 24, 2019
November 24, 2019By MedStar Health Research Institute
Join us in congratulating Cristiane Gomes-Lima, MD, on her 2019 Women Advancing Thyroid Research (WATR) award from the American Thyroid Association (ATA). The WATR is a new award from the Ameri...
-
 November 22, 2019
November 22, 2019By Jasmeet Singh Bhogal, MD, MBA
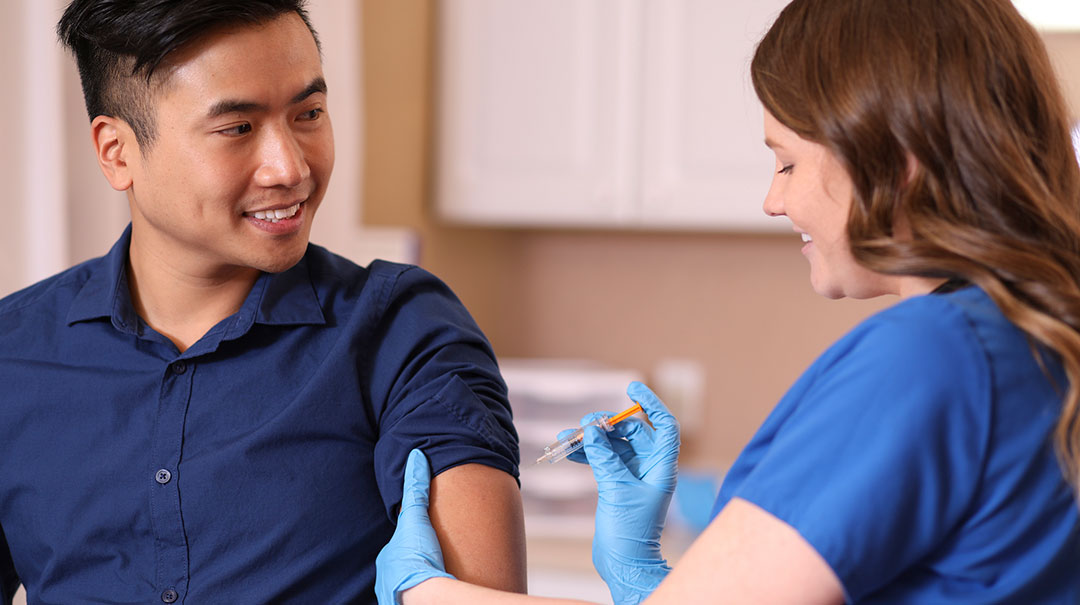
Cold weather is upon us—and, unfortunately, so is flu season. The flu, which is most common in the fall and winter, is a contagious respiratory illness that’s caused by a virus called influenza. The m...
-
 November 15, 2019
November 15, 2019Seizures, or changes in the brain’s electrical activity, are more common than most people realize—in fact, about one in 100 Americans have had an unprovoked seizure and one in 26 people will develop e...
-
 November 02, 2019
November 02, 2019By MedStar Health Research Institute
Congratulations to all MedStar researchers who had articles published in October 2019. The selected articles and link to PubMed provided below represent the body of work completed by MedStar Health in...
- 1
- 2
- 3
- 4
- 5
- 6
- 7
- 8
- 9
- 10
- 11
- 12
- 13
- 14
- 15
- 16
- 17
- 18
- 19
- 20
- 21
- 22
- 23
- 24
- 25
- 26
- 27
- 28
- 29
- 30
- 31
- 32
- 33
- 34
- 35
- 36
- 37
- 38
- 39
- 40
- 41
- 42
- 43
- 44
- 45
- 46
- 47
- 48
- 49
- 50
- 51
- 52
- 53
- 54
- 55
- 56
- 57
- 58
- 59
- 60
- 61
- 62
- 63
- 64
- 65
- 66
- 67
- 68
- 69
- 70
- 71
- 72
- 73
- 74
- 75
- 76
- 77
- 78
- 79
- 80
- 81
- 82
- 83
- 84
- 85
- 86
- 87
- 88
- 89
- 90
- 91
- 92
- 93
- 94
- 95
- 96
- 97
- 98
- 99
- 100
- 101
- 102
- 103
- 104
- 105
- 106
- 107
- 108
- 109
- 110
- 111
- 112
- 113
- 114
- 115
- 116
- 117
- 118
- 119
- 120
- 121
- 122
- 123
- 124
- 125
- 126
- 127
- 128
- 129
- 130
- 131
- 132
- 133
- 134
- 135
- 136
- 137
- 138
- 139
- 140
- 141
- 142
- 143
- 144
- 145
- 146
- 147
- 148
- 149
- 150
- 151
- 152
- 153
- 154
- 155
- 156
- 157
- 158
- 159
- 160
- 161
- 162
- 163
- 164
- 165
- 166
- 167
- 168
- 169
- 170
- 171
- 172
- 173
- 174
- 175
- 176
- 177
- 178
- 179
- 180
- 181
- 182
- 183
- 184
- 185
- 186
- 187
- 188
- 189
- 190
- 191
- 192
- 193
- 194
- 195
- 196
- 197
- 198
- 199
- 200
- 201
- 202
- 203
- 204
- 205
- 206
- 207
- 208
- 209
- 210
- 211
- 212
- 213
- 214
- 215
- 216
- 217
- 218
- 219
- 220
- 221
- 222
- 223
- 224
- 225
- 226
- 227
- 228
- 229
- 230
- 231
- 232
- 233
- 234
- 235
- 236
- 237
- 238
- 239
- 240
- 241
- 242
- 243
- 244
- 245
- 246
- 247
- 248
- 249
- 250
- 251
- 252
- 253
- 254
- 255
- 256
- 257
- 258
- 259
- 260
- 261
- 262
- 263
- 264
- 265
- 266
- 267
- 268
- 269
- 270
- 271
- 272
- 273
- 274
- 275
- 276
- 277
- 278
- 279
- 280
- 281
- 282
- 283
- 284
- 285
- 286
- 287
- 288
- 289
- 290
- 291
- 292
- 293
- 294
- 295
- 296
- 297
- 298
- 299
- 300
- 301










