Featured Blog
-
 May 27, 2026
May 27, 2026As a sports performance coach, one of the biggest things I come back to is this: our world has become a highlight reel. Social media has changed how athletes see training, progress, and even the...
Browse blogs by hospital
Share this
All Blogs
-
August 07, 2019
Insomnia is habitual sleeplessness or the inability to sleep that isn’t explained by a medical condition (i.e. sleep apnea). It includes your habits or schedule causing you to not get enough sleep or ...
-
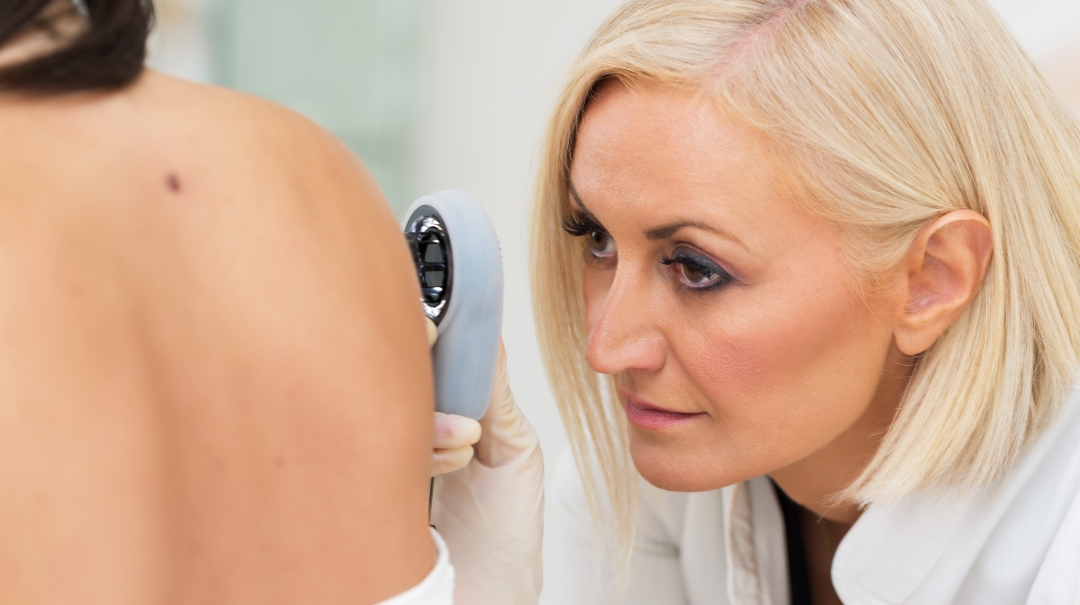 August 05, 2019
August 05, 2019Our skin is a sensitive organ that can be affected by the outside world, such as the UV rays produced by the sun. Skin cancer—the most common type of cancer in America—can be caused by the sun, causi...
-
 August 02, 2019
August 02, 2019“When you wake up in the morning, Pooh," said Piglet at last, "what's the first thing you say to yourself?" "What's for breakfast?" said Pooh. "What do you say, Piglet?""I say, I wonder what's going ...
-
 August 02, 2019
August 02, 2019By MedStar Health Research Institute
The mission of the Association for Academic Surgery is to inspire and develop young academic surgeonsRegister now for the 2019 Association for Academic Surgery fall courses. These courses will take pl...
-
 August 02, 2019
August 02, 2019By MedStar Health Research Institute
Join more than 3,000 interventional and endovascular specialists at Cardiovascular Research Technologies Conference (CRT) 2020 for a comprehensive four-day interventional cardiology conference featuri...
-
 August 02, 2019
August 02, 2019By MedStar Health Research Institute
Mark your calendars now to connect with other MHRI and MedStar associates by participating in one of these upcoming events to support the health of our communities. Race to Beat Cancer Saturday, Septe...
- 1
- 2
- 3
- 4
- 5
- 6
- 7
- 8
- 9
- 10
- 11
- 12
- 13
- 14
- 15
- 16
- 17
- 18
- 19
- 20
- 21
- 22
- 23
- 24
- 25
- 26
- 27
- 28
- 29
- 30
- 31
- 32
- 33
- 34
- 35
- 36
- 37
- 38
- 39
- 40
- 41
- 42
- 43
- 44
- 45
- 46
- 47
- 48
- 49
- 50
- 51
- 52
- 53
- 54
- 55
- 56
- 57
- 58
- 59
- 60
- 61
- 62
- 63
- 64
- 65
- 66
- 67
- 68
- 69
- 70
- 71
- 72
- 73
- 74
- 75
- 76
- 77
- 78
- 79
- 80
- 81
- 82
- 83
- 84
- 85
- 86
- 87
- 88
- 89
- 90
- 91
- 92
- 93
- 94
- 95
- 96
- 97
- 98
- 99
- 100
- 101
- 102
- 103
- 104
- 105
- 106
- 107
- 108
- 109
- 110
- 111
- 112
- 113
- 114
- 115
- 116
- 117
- 118
- 119
- 120
- 121
- 122
- 123
- 124
- 125
- 126
- 127
- 128
- 129
- 130
- 131
- 132
- 133
- 134
- 135
- 136
- 137
- 138
- 139
- 140
- 141
- 142
- 143
- 144
- 145
- 146
- 147
- 148
- 149
- 150
- 151
- 152
- 153
- 154
- 155
- 156
- 157
- 158
- 159
- 160
- 161
- 162
- 163
- 164
- 165
- 166
- 167
- 168
- 169
- 170
- 171
- 172
- 173
- 174
- 175
- 176
- 177
- 178
- 179
- 180
- 181
- 182
- 183
- 184
- 185
- 186
- 187
- 188
- 189
- 190
- 191
- 192
- 193
- 194
- 195
- 196
- 197
- 198
- 199
- 200
- 201
- 202
- 203
- 204
- 205
- 206
- 207
- 208
- 209
- 210
- 211
- 212
- 213
- 214
- 215
- 216
- 217
- 218
- 219
- 220
- 221
- 222
- 223
- 224
- 225
- 226
- 227
- 228
- 229
- 230
- 231
- 232
- 233
- 234
- 235
- 236
- 237
- 238
- 239
- 240
- 241
- 242
- 243
- 244
- 245
- 246
- 247
- 248
- 249
- 250
- 251
- 252
- 253
- 254
- 255
- 256
- 257
- 258
- 259
- 260
- 261
- 262
- 263
- 264
- 265
- 266
- 267
- 268
- 269
- 270
- 271
- 272
- 273
- 274
- 275
- 276
- 277
- 278
- 279
- 280
- 281
- 282
- 283
- 284
- 285
- 286
- 287
- 288
- 289
- 290
- 291
- 292
- 293
- 294
- 295
- 296
- 297
- 298
- 299
- 300
- 301
- 302










