Featured Blog
-
 May 22, 2026
May 22, 2026By MedStar Team
This article was written by James Howard Street III, MD and Ian Weston, AVP of Operations. A split second can be all it takes for a routine afternoon to turn into a life-altering event. W...
Browse blogs by hospital
Share this
All Blogs
-
 January 23, 2019
January 23, 2019Many parents are cautious to protect their children against seasonal illnesses, such as colds and the flu. However, a lesser-known viral infection called hand, foot, and mouth disease, is also promine...
-
 January 22, 2019
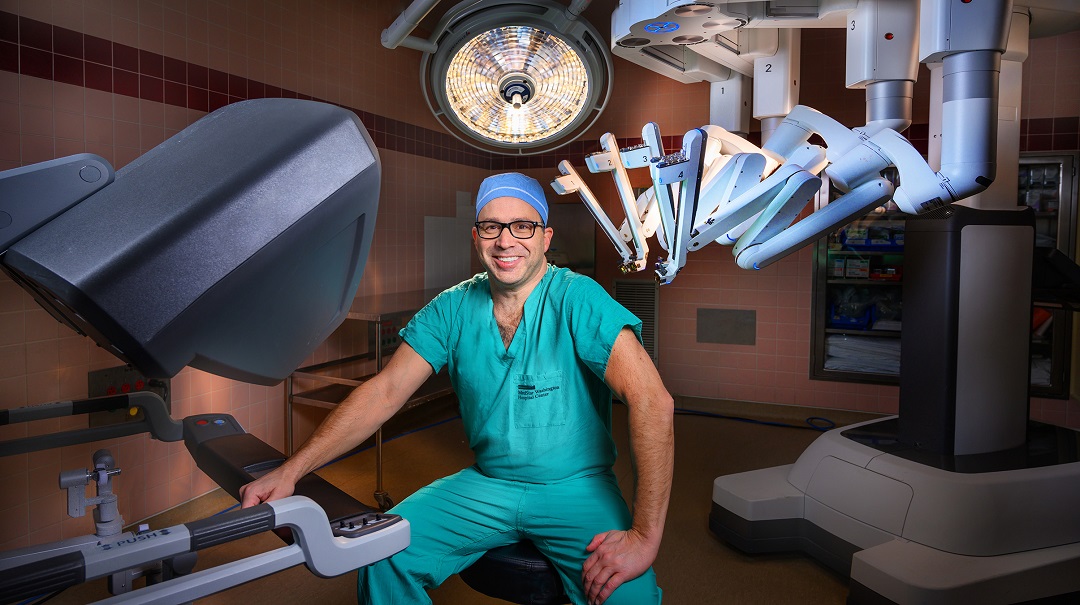
January 22, 2019When the first minimally invasive surgery—also called laparoscopic surgery—was performed in the early 1900s, a surgeon would use a hollow wooden tube with a candle to look in a patient&r...
-
 January 18, 2019
January 18, 2019Some days it’s hard enough just to find the energy to make it out of bed and into work on time. Eating healthy can often end up feeling almost impossible combined with all of the other items you need ...
-
 January 15, 2019
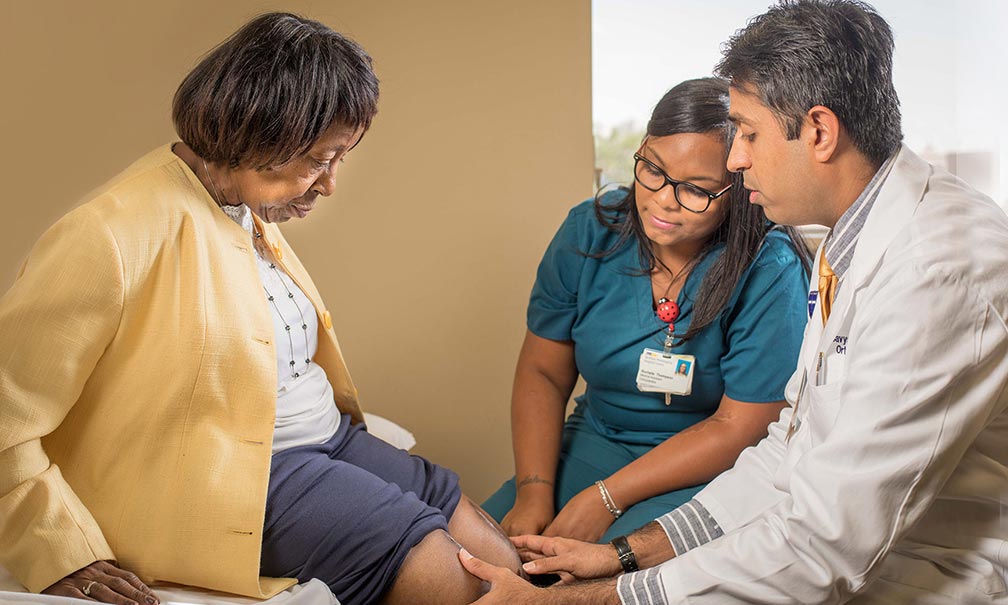
January 15, 2019Total joint replacement, comprised of hip or knee replacements, is one of the most common surgical procedures in the U.S. These devices have given millions of people continued or increased activity a...
-
January 09, 2019
Running a 5K is a challenging and fun way to stay fit. Although, if you aren’t careful, you can get injured while training or during the event. As 5Ks become more and more popular, we&rsq...
-
 January 08, 2019
January 08, 2019A vasectomy is one way men can prevent their partners from becoming pregnant—without affecting sexual function or the ability to orgasm. A vasectomy is a noninvasive surgery that prohibits sper...
- 1
- 2
- 3
- 4
- 5
- 6
- 7
- 8
- 9
- 10
- 11
- 12
- 13
- 14
- 15
- 16
- 17
- 18
- 19
- 20
- 21
- 22
- 23
- 24
- 25
- 26
- 27
- 28
- 29
- 30
- 31
- 32
- 33
- 34
- 35
- 36
- 37
- 38
- 39
- 40
- 41
- 42
- 43
- 44
- 45
- 46
- 47
- 48
- 49
- 50
- 51
- 52
- 53
- 54
- 55
- 56
- 57
- 58
- 59
- 60
- 61
- 62
- 63
- 64
- 65
- 66
- 67
- 68
- 69
- 70
- 71
- 72
- 73
- 74
- 75
- 76
- 77
- 78
- 79
- 80
- 81
- 82
- 83
- 84
- 85
- 86
- 87
- 88
- 89
- 90
- 91
- 92
- 93
- 94
- 95
- 96
- 97
- 98
- 99
- 100
- 101
- 102
- 103
- 104
- 105
- 106
- 107
- 108
- 109
- 110
- 111
- 112
- 113
- 114
- 115
- 116
- 117
- 118
- 119
- 120
- 121
- 122
- 123
- 124
- 125
- 126
- 127
- 128
- 129
- 130
- 131
- 132
- 133
- 134
- 135
- 136
- 137
- 138
- 139
- 140
- 141
- 142
- 143
- 144
- 145
- 146
- 147
- 148
- 149
- 150
- 151
- 152
- 153
- 154
- 155
- 156
- 157
- 158
- 159
- 160
- 161
- 162
- 163
- 164
- 165
- 166
- 167
- 168
- 169
- 170
- 171
- 172
- 173
- 174
- 175
- 176
- 177
- 178
- 179
- 180
- 181
- 182
- 183
- 184
- 185
- 186
- 187
- 188
- 189
- 190
- 191
- 192
- 193
- 194
- 195
- 196
- 197
- 198
- 199
- 200
- 201
- 202
- 203
- 204
- 205
- 206
- 207
- 208
- 209
- 210
- 211
- 212
- 213
- 214
- 215
- 216
- 217
- 218
- 219
- 220
- 221
- 222
- 223
- 224
- 225
- 226
- 227
- 228
- 229
- 230
- 231
- 232
- 233
- 234
- 235
- 236
- 237
- 238
- 239
- 240
- 241
- 242
- 243
- 244
- 245
- 246
- 247
- 248
- 249
- 250
- 251
- 252
- 253
- 254
- 255
- 256
- 257
- 258
- 259
- 260
- 261
- 262
- 263
- 264
- 265
- 266
- 267
- 268
- 269
- 270
- 271
- 272
- 273
- 274
- 275
- 276
- 277
- 278
- 279
- 280
- 281
- 282
- 283
- 284
- 285
- 286
- 287
- 288
- 289
- 290
- 291
- 292
- 293
- 294
- 295
- 296
- 297
- 298
- 299
- 300
- 301










