Featured Blog
-
 May 22, 2026
May 22, 2026By MedStar Team
This article was written by James Howard Street III, MD and Ian Weston, AVP of Operations. A split second can be all it takes for a routine afternoon to turn into a life-altering event. W...
Browse blogs by hospital
Share this
All Blogs
-
 April 05, 2019
April 05, 2019Having a healthy heart is pivotal, as heart disease is the leading cause of death in the U.S. This is especially important once you get into your 30s, as heart disease risk increases with age. ...
-
 April 05, 2019
April 05, 2019By MedStar Health Research Institute
MedStar Health strives to provide associates with the tools and learning opportunities to succeed in the ever-changing healthcare industry. To accomplish this, associates are encouraged to take advant...
-
 April 05, 2019
April 05, 2019By MedStar Health Research Institute
Applications are now being accepted for the Pilot Awards for Clinical Translational Studies (PTCS) through GHUCCTS. Applications Submissions are online at PTCS Applications. The completed application...
-
 April 05, 2019
April 05, 2019By MedStar Health Research Institute
At MedStar Health, we are committed to creating an academic healthcare system that fosters and supports research. To support this effort, we are pleased to announce two (2) intramural grant fu...
-
 April 05, 2019
April 05, 2019By MedStar Health Research Institute
Organized by the Department of Continuing Professional Education, MedStar Health is offering a variety of CE conferences this spring that provide an opportunity to gain knowledge of new treatments and...
-
 April 04, 2019
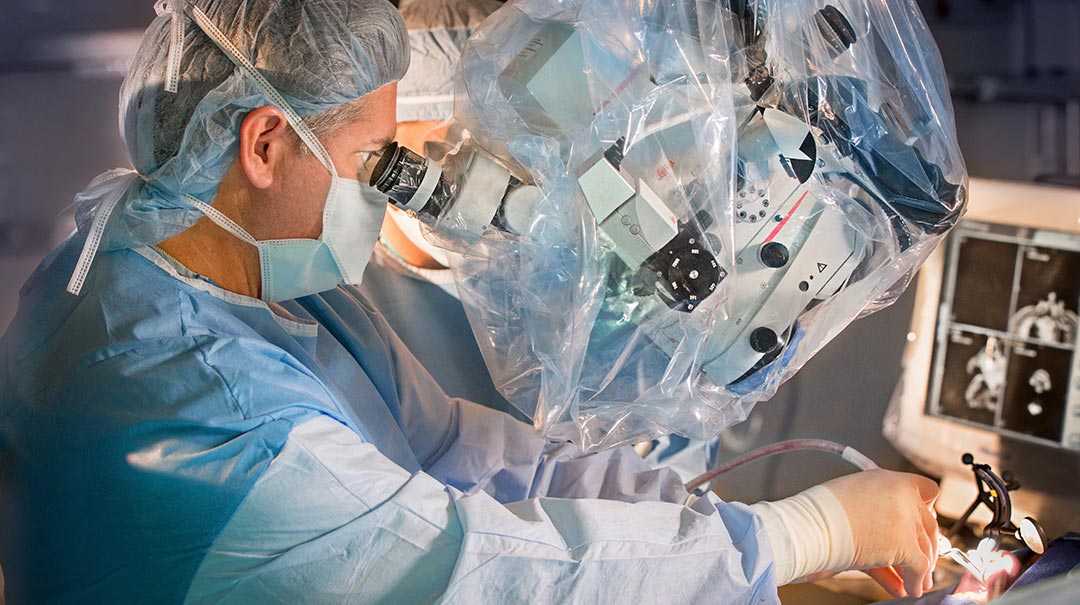
April 04, 2019Imagine this scenario: You come to the hospital with a complex neurological condition, and your surgeon uses a device or instrument you’ve never seen before—a tool that is perfectly designed to approa...
- 1
- 2
- 3
- 4
- 5
- 6
- 7
- 8
- 9
- 10
- 11
- 12
- 13
- 14
- 15
- 16
- 17
- 18
- 19
- 20
- 21
- 22
- 23
- 24
- 25
- 26
- 27
- 28
- 29
- 30
- 31
- 32
- 33
- 34
- 35
- 36
- 37
- 38
- 39
- 40
- 41
- 42
- 43
- 44
- 45
- 46
- 47
- 48
- 49
- 50
- 51
- 52
- 53
- 54
- 55
- 56
- 57
- 58
- 59
- 60
- 61
- 62
- 63
- 64
- 65
- 66
- 67
- 68
- 69
- 70
- 71
- 72
- 73
- 74
- 75
- 76
- 77
- 78
- 79
- 80
- 81
- 82
- 83
- 84
- 85
- 86
- 87
- 88
- 89
- 90
- 91
- 92
- 93
- 94
- 95
- 96
- 97
- 98
- 99
- 100
- 101
- 102
- 103
- 104
- 105
- 106
- 107
- 108
- 109
- 110
- 111
- 112
- 113
- 114
- 115
- 116
- 117
- 118
- 119
- 120
- 121
- 122
- 123
- 124
- 125
- 126
- 127
- 128
- 129
- 130
- 131
- 132
- 133
- 134
- 135
- 136
- 137
- 138
- 139
- 140
- 141
- 142
- 143
- 144
- 145
- 146
- 147
- 148
- 149
- 150
- 151
- 152
- 153
- 154
- 155
- 156
- 157
- 158
- 159
- 160
- 161
- 162
- 163
- 164
- 165
- 166
- 167
- 168
- 169
- 170
- 171
- 172
- 173
- 174
- 175
- 176
- 177
- 178
- 179
- 180
- 181
- 182
- 183
- 184
- 185
- 186
- 187
- 188
- 189
- 190
- 191
- 192
- 193
- 194
- 195
- 196
- 197
- 198
- 199
- 200
- 201
- 202
- 203
- 204
- 205
- 206
- 207
- 208
- 209
- 210
- 211
- 212
- 213
- 214
- 215
- 216
- 217
- 218
- 219
- 220
- 221
- 222
- 223
- 224
- 225
- 226
- 227
- 228
- 229
- 230
- 231
- 232
- 233
- 234
- 235
- 236
- 237
- 238
- 239
- 240
- 241
- 242
- 243
- 244
- 245
- 246
- 247
- 248
- 249
- 250
- 251
- 252
- 253
- 254
- 255
- 256
- 257
- 258
- 259
- 260
- 261
- 262
- 263
- 264
- 265
- 266
- 267
- 268
- 269
- 270
- 271
- 272
- 273
- 274
- 275
- 276
- 277
- 278
- 279
- 280
- 281
- 282
- 283
- 284
- 285
- 286
- 287
- 288
- 289
- 290
- 291
- 292
- 293
- 294
- 295
- 296
- 297
- 298
- 299
- 300
- 301










