Featured Blog
-
 May 22, 2026
May 22, 2026By MedStar Team
This article was written by James Howard Street III, MD and Ian Weston, AVP of Operations. A split second can be all it takes for a routine afternoon to turn into a life-altering event. W...
Browse blogs by hospital
Share this
All Blogs
-
January 29, 2021
As the COVID-19 vaccine becomes available across the nation, you may have some questions about whether or not you should get vaccinated. In part one of this series on frequently asked questions a...
-
January 28, 2021
Did you know that bladder cancer is the fourth most common non-skin cancer in the U.S.? Unlike prostate cancer, for which there is a standard screening, bladder cancer can frequently fall under t...
-
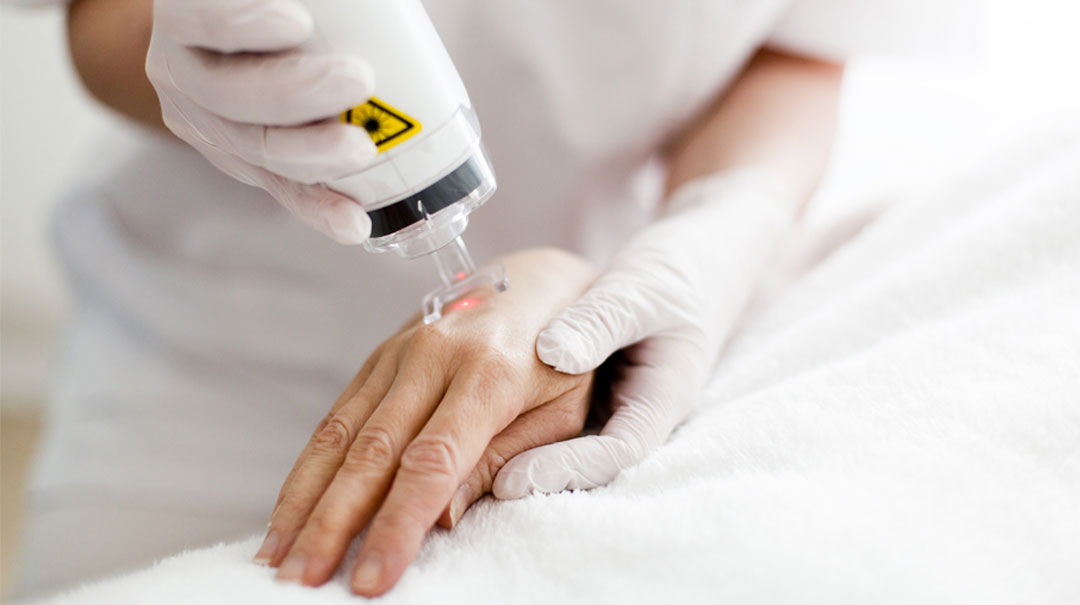 January 26, 2021
January 26, 2021Whatever the cause—burns, trauma or surgery—scars can have a negative impact on a patient’s quality of life. In decades past, treatment of symptomatic scarring (scars that result i...
-
January 21, 2021
As a former service member in the Army, I’m no stranger to vaccines. And today, as an infectious disease specialist, I’m grateful to be protected against the coronavirus after receiving the COVID...
-
 January 21, 2021
January 21, 2021By MedStar Team
Skiing, skating and sledding can be great wintertime fun. But the elements that bring the greatest thrill to these sports—gravity, speed and ice—can also make them quite dangerous. Sport...
-
January 20, 2021
By MedStar Team
When you have chronic pain that gets in the way of everyday activities, you may benefit from pain management treatment. Not all pain management clinics offer the same options that can improve your q...
- 1
- 2
- 3
- 4
- 5
- 6
- 7
- 8
- 9
- 10
- 11
- 12
- 13
- 14
- 15
- 16
- 17
- 18
- 19
- 20
- 21
- 22
- 23
- 24
- 25
- 26
- 27
- 28
- 29
- 30
- 31
- 32
- 33
- 34
- 35
- 36
- 37
- 38
- 39
- 40
- 41
- 42
- 43
- 44
- 45
- 46
- 47
- 48
- 49
- 50
- 51
- 52
- 53
- 54
- 55
- 56
- 57
- 58
- 59
- 60
- 61
- 62
- 63
- 64
- 65
- 66
- 67
- 68
- 69
- 70
- 71
- 72
- 73
- 74
- 75
- 76
- 77
- 78
- 79
- 80
- 81
- 82
- 83
- 84
- 85
- 86
- 87
- 88
- 89
- 90
- 91
- 92
- 93
- 94
- 95
- 96
- 97
- 98
- 99
- 100
- 101
- 102
- 103
- 104
- 105
- 106
- 107
- 108
- 109
- 110
- 111
- 112
- 113
- 114
- 115
- 116
- 117
- 118
- 119
- 120
- 121
- 122
- 123
- 124
- 125
- 126
- 127
- 128
- 129
- 130
- 131
- 132
- 133
- 134
- 135
- 136
- 137
- 138
- 139
- 140
- 141
- 142
- 143
- 144
- 145
- 146
- 147
- 148
- 149
- 150
- 151
- 152
- 153
- 154
- 155
- 156
- 157
- 158
- 159
- 160
- 161
- 162
- 163
- 164
- 165
- 166
- 167
- 168
- 169
- 170
- 171
- 172
- 173
- 174
- 175
- 176
- 177
- 178
- 179
- 180
- 181
- 182
- 183
- 184
- 185
- 186
- 187
- 188
- 189
- 190
- 191
- 192
- 193
- 194
- 195
- 196
- 197
- 198
- 199
- 200
- 201
- 202
- 203
- 204
- 205
- 206
- 207
- 208
- 209
- 210
- 211
- 212
- 213
- 214
- 215
- 216
- 217
- 218
- 219
- 220
- 221
- 222
- 223
- 224
- 225
- 226
- 227
- 228
- 229
- 230
- 231
- 232
- 233
- 234
- 235
- 236
- 237
- 238
- 239
- 240
- 241
- 242
- 243
- 244
- 245
- 246
- 247
- 248
- 249
- 250
- 251
- 252
- 253
- 254
- 255
- 256
- 257
- 258
- 259
- 260
- 261
- 262
- 263
- 264
- 265
- 266
- 267
- 268
- 269
- 270
- 271
- 272
- 273
- 274
- 275
- 276
- 277
- 278
- 279
- 280
- 281
- 282
- 283
- 284
- 285
- 286
- 287
- 288
- 289
- 290
- 291
- 292
- 293
- 294
- 295
- 296
- 297
- 298
- 299
- 300
- 301










