Featured Blog
-
 May 26, 2026
May 26, 2026Our research, published in the Journal of Cancer Survivorship, helps us understand the risk of functional limitations after cancer treatment, enabling us to improve care for survivors. There are ma...
Browse blogs by hospital
Share this
All Blogs
-
 August 01, 2020
August 01, 2020By MedStar Team
Congratulations to all MedStar researchers who had articles published in July 2020. The selected articles and link to PubMed provided below represent the body of work completed by MedStar Health inves...
-
August 01, 2020
By MedStar Health Research Institute
As of July 1, 2020, a single COI platform is available to all Researchers employed by MedStar Health (to include those located at MedStar Georgetown University Hospital (“MGUH”) or elsewhe...
-
July 31, 2020
If you’re pregnant, you may have some questions about what’s next. Many women feel a mix of emotions, which is why it’s important to have a care team to guide you every stage of your journey to a heal...
-
 July 31, 2020
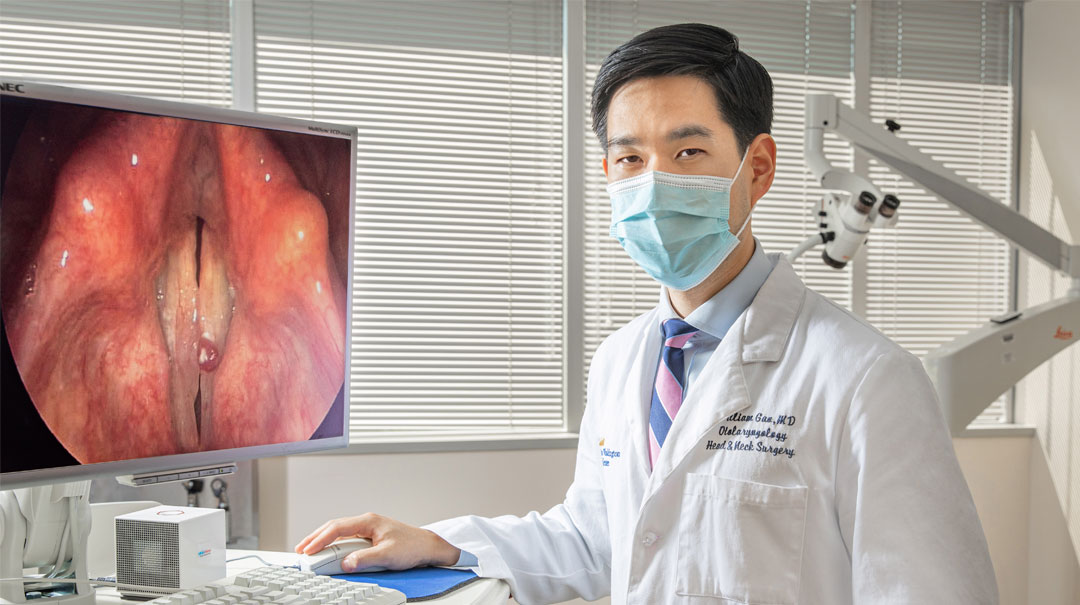
July 31, 2020By MedStar Team
When we face losing our voice, we may feel challenged not just functionally but emotionally as well. Our natural way of communicating—something most of us take for granted—is interrupted,...
-
 July 29, 2020
July 29, 2020For centuries, women who experience severe menstrual pain have been told that the discomfort is just part of being a woman. It’s not. This level of pain could be endometriosis, and a woman who ...
-
July 27, 2020
By MedStar Team
While infants and kids can catch COVID-19, fewer than 5 percent of reported cases in the U.S. occur in children. And, kids that do catch the virus typically demonstrate much milder symptoms than adult...
- 1
- 2
- 3
- 4
- 5
- 6
- 7
- 8
- 9
- 10
- 11
- 12
- 13
- 14
- 15
- 16
- 17
- 18
- 19
- 20
- 21
- 22
- 23
- 24
- 25
- 26
- 27
- 28
- 29
- 30
- 31
- 32
- 33
- 34
- 35
- 36
- 37
- 38
- 39
- 40
- 41
- 42
- 43
- 44
- 45
- 46
- 47
- 48
- 49
- 50
- 51
- 52
- 53
- 54
- 55
- 56
- 57
- 58
- 59
- 60
- 61
- 62
- 63
- 64
- 65
- 66
- 67
- 68
- 69
- 70
- 71
- 72
- 73
- 74
- 75
- 76
- 77
- 78
- 79
- 80
- 81
- 82
- 83
- 84
- 85
- 86
- 87
- 88
- 89
- 90
- 91
- 92
- 93
- 94
- 95
- 96
- 97
- 98
- 99
- 100
- 101
- 102
- 103
- 104
- 105
- 106
- 107
- 108
- 109
- 110
- 111
- 112
- 113
- 114
- 115
- 116
- 117
- 118
- 119
- 120
- 121
- 122
- 123
- 124
- 125
- 126
- 127
- 128
- 129
- 130
- 131
- 132
- 133
- 134
- 135
- 136
- 137
- 138
- 139
- 140
- 141
- 142
- 143
- 144
- 145
- 146
- 147
- 148
- 149
- 150
- 151
- 152
- 153
- 154
- 155
- 156
- 157
- 158
- 159
- 160
- 161
- 162
- 163
- 164
- 165
- 166
- 167
- 168
- 169
- 170
- 171
- 172
- 173
- 174
- 175
- 176
- 177
- 178
- 179
- 180
- 181
- 182
- 183
- 184
- 185
- 186
- 187
- 188
- 189
- 190
- 191
- 192
- 193
- 194
- 195
- 196
- 197
- 198
- 199
- 200
- 201
- 202
- 203
- 204
- 205
- 206
- 207
- 208
- 209
- 210
- 211
- 212
- 213
- 214
- 215
- 216
- 217
- 218
- 219
- 220
- 221
- 222
- 223
- 224
- 225
- 226
- 227
- 228
- 229
- 230
- 231
- 232
- 233
- 234
- 235
- 236
- 237
- 238
- 239
- 240
- 241
- 242
- 243
- 244
- 245
- 246
- 247
- 248
- 249
- 250
- 251
- 252
- 253
- 254
- 255
- 256
- 257
- 258
- 259
- 260
- 261
- 262
- 263
- 264
- 265
- 266
- 267
- 268
- 269
- 270
- 271
- 272
- 273
- 274
- 275
- 276
- 277
- 278
- 279
- 280
- 281
- 282
- 283
- 284
- 285
- 286
- 287
- 288
- 289
- 290
- 291
- 292
- 293
- 294
- 295
- 296
- 297
- 298
- 299
- 300
- 301










