Featured Blog
-
 May 26, 2026
May 26, 2026Our research, published in the Journal of Cancer Survivorship, helps us understand the risk of functional limitations after cancer treatment, enabling us to improve care for survivors. There are ma...
Browse blogs by hospital
Share this
All Blogs
-
 January 08, 2019
January 08, 2019A vasectomy is one way men can prevent their partners from becoming pregnant—without affecting sexual function or the ability to orgasm. A vasectomy is a noninvasive surgery that prohibits sper...
-
 January 07, 2019
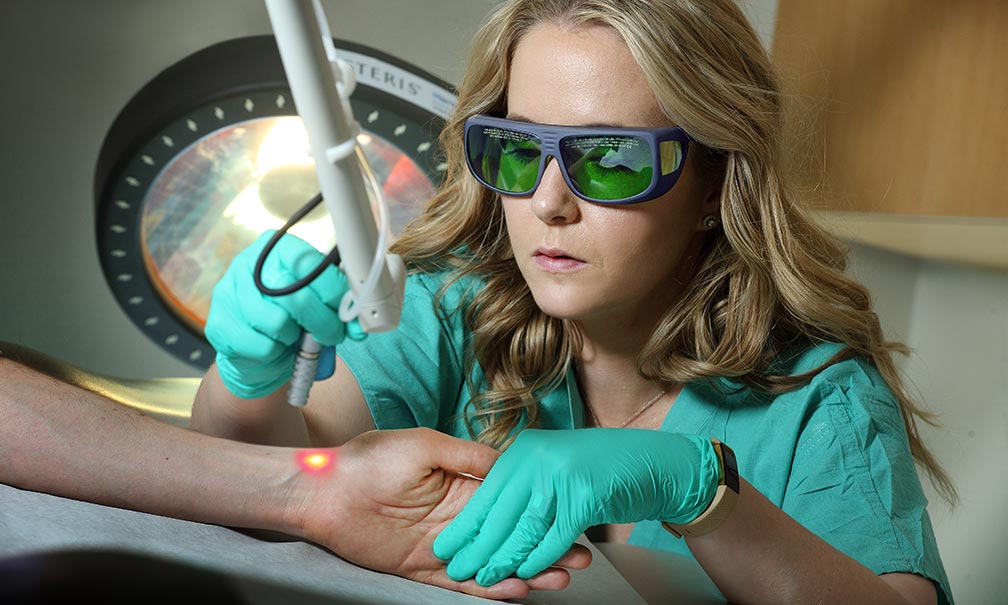
January 07, 2019It might seem unusual at first to think of a doctor using laser therapy to treat a burn injury scar. Why would burning the body’s tissue further help a patient heal? But lasers are an extremely valuab...
-
 January 04, 2019
January 04, 2019Every year, thousands of runners across the U.S. complete 5K races, which is equivalent to 3.1 miles. Most people who are new to running shouldn’t just step out the door and attempt to run...
-
 January 04, 2019
January 04, 2019By MedStar Health Research Institute
Research Grand Rounds: Translational Science Approaches to the Study of Aging and Neuroinflammation—February 1, 2019Research Grand Rounds are sponsored by MedStar Health Research Institute and Georget...
-
 January 04, 2019
January 04, 2019By MedStar Health Research Institute
We are pleased to announce the 2019-2021 cohorts of the MedStar Health Research and Teaching Scholars! The MedStar Research Scholars program supports the development of MedStar clinici...
-
 January 04, 2019
January 04, 2019By MedStar Health Research Institute
In December, MHRI associates took some time out of their busy schedules to celebrate the successes of 2018 with their fellow associates. These events are also our opportunity to recognize associ...
- 1
- 2
- 3
- 4
- 5
- 6
- 7
- 8
- 9
- 10
- 11
- 12
- 13
- 14
- 15
- 16
- 17
- 18
- 19
- 20
- 21
- 22
- 23
- 24
- 25
- 26
- 27
- 28
- 29
- 30
- 31
- 32
- 33
- 34
- 35
- 36
- 37
- 38
- 39
- 40
- 41
- 42
- 43
- 44
- 45
- 46
- 47
- 48
- 49
- 50
- 51
- 52
- 53
- 54
- 55
- 56
- 57
- 58
- 59
- 60
- 61
- 62
- 63
- 64
- 65
- 66
- 67
- 68
- 69
- 70
- 71
- 72
- 73
- 74
- 75
- 76
- 77
- 78
- 79
- 80
- 81
- 82
- 83
- 84
- 85
- 86
- 87
- 88
- 89
- 90
- 91
- 92
- 93
- 94
- 95
- 96
- 97
- 98
- 99
- 100
- 101
- 102
- 103
- 104
- 105
- 106
- 107
- 108
- 109
- 110
- 111
- 112
- 113
- 114
- 115
- 116
- 117
- 118
- 119
- 120
- 121
- 122
- 123
- 124
- 125
- 126
- 127
- 128
- 129
- 130
- 131
- 132
- 133
- 134
- 135
- 136
- 137
- 138
- 139
- 140
- 141
- 142
- 143
- 144
- 145
- 146
- 147
- 148
- 149
- 150
- 151
- 152
- 153
- 154
- 155
- 156
- 157
- 158
- 159
- 160
- 161
- 162
- 163
- 164
- 165
- 166
- 167
- 168
- 169
- 170
- 171
- 172
- 173
- 174
- 175
- 176
- 177
- 178
- 179
- 180
- 181
- 182
- 183
- 184
- 185
- 186
- 187
- 188
- 189
- 190
- 191
- 192
- 193
- 194
- 195
- 196
- 197
- 198
- 199
- 200
- 201
- 202
- 203
- 204
- 205
- 206
- 207
- 208
- 209
- 210
- 211
- 212
- 213
- 214
- 215
- 216
- 217
- 218
- 219
- 220
- 221
- 222
- 223
- 224
- 225
- 226
- 227
- 228
- 229
- 230
- 231
- 232
- 233
- 234
- 235
- 236
- 237
- 238
- 239
- 240
- 241
- 242
- 243
- 244
- 245
- 246
- 247
- 248
- 249
- 250
- 251
- 252
- 253
- 254
- 255
- 256
- 257
- 258
- 259
- 260
- 261
- 262
- 263
- 264
- 265
- 266
- 267
- 268
- 269
- 270
- 271
- 272
- 273
- 274
- 275
- 276
- 277
- 278
- 279
- 280
- 281
- 282
- 283
- 284
- 285
- 286
- 287
- 288
- 289
- 290
- 291
- 292
- 293
- 294
- 295
- 296
- 297
- 298
- 299
- 300
- 301










