Featured Blog
-
 May 22, 2026
May 22, 2026By MedStar Team
This article was written by James Howard Street III, MD and Ian Weston, AVP of Operations. A split second can be all it takes for a routine afternoon to turn into a life-altering event. W...
Browse blogs by hospital
Share this
All Blogs
-
 March 29, 2018
March 29, 2018By MedStar Health Research Institute
Research Grand Rounds are sponsored by MedStar Health Research Institute and Georgetown-Howard Universities Center for Clinical and Translational Science (GHUCCTS) and bring together the MedStar Heal...
-
 March 29, 2018
March 29, 2018By MedStar Health Research Institute
A guest post from Christina Stanger, MA, CRA, Director of the MHRI Office of Contract and Grant ManagementDo you present at conferences in your specialty area? How about your staff? Presenting at prof...
-
 March 29, 2018
March 29, 2018A diagnosis of heart failure doesn’t mean your heart has stopped or is about to stop working. It’s a condition in which the heart cannot adequately pump blood to the body. Heart fail...
-
 March 29, 2018
March 29, 2018By MedStar Health Research Institute
Congratulations to all MedStar researchers who had articles published in March 2018. The selected articles and link to PubMed provided below represent the body of work completed by MedStar Health inve...
-
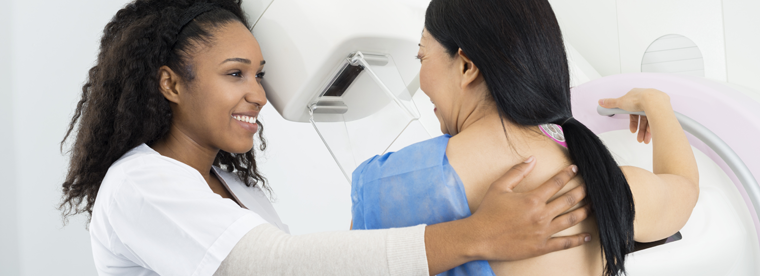 March 29, 2018
March 29, 2018By MedStar Health Research Institute
Educational intervention by community health workers was found to have a positive impact on perceptions of mammogram safety and efficacy in breast health and cancer awareness, recent research from the...
-
 March 29, 2018
March 29, 2018By MedStar Health Research Institute
Multi-site research studies funded by the National Institutes of Health (NIH) are required to use a single IRB of record for all participating sites. This policy applies to non-exempt human subjects r...
- 1
- 2
- 3
- 4
- 5
- 6
- 7
- 8
- 9
- 10
- 11
- 12
- 13
- 14
- 15
- 16
- 17
- 18
- 19
- 20
- 21
- 22
- 23
- 24
- 25
- 26
- 27
- 28
- 29
- 30
- 31
- 32
- 33
- 34
- 35
- 36
- 37
- 38
- 39
- 40
- 41
- 42
- 43
- 44
- 45
- 46
- 47
- 48
- 49
- 50
- 51
- 52
- 53
- 54
- 55
- 56
- 57
- 58
- 59
- 60
- 61
- 62
- 63
- 64
- 65
- 66
- 67
- 68
- 69
- 70
- 71
- 72
- 73
- 74
- 75
- 76
- 77
- 78
- 79
- 80
- 81
- 82
- 83
- 84
- 85
- 86
- 87
- 88
- 89
- 90
- 91
- 92
- 93
- 94
- 95
- 96
- 97
- 98
- 99
- 100
- 101
- 102
- 103
- 104
- 105
- 106
- 107
- 108
- 109
- 110
- 111
- 112
- 113
- 114
- 115
- 116
- 117
- 118
- 119
- 120
- 121
- 122
- 123
- 124
- 125
- 126
- 127
- 128
- 129
- 130
- 131
- 132
- 133
- 134
- 135
- 136
- 137
- 138
- 139
- 140
- 141
- 142
- 143
- 144
- 145
- 146
- 147
- 148
- 149
- 150
- 151
- 152
- 153
- 154
- 155
- 156
- 157
- 158
- 159
- 160
- 161
- 162
- 163
- 164
- 165
- 166
- 167
- 168
- 169
- 170
- 171
- 172
- 173
- 174
- 175
- 176
- 177
- 178
- 179
- 180
- 181
- 182
- 183
- 184
- 185
- 186
- 187
- 188
- 189
- 190
- 191
- 192
- 193
- 194
- 195
- 196
- 197
- 198
- 199
- 200
- 201
- 202
- 203
- 204
- 205
- 206
- 207
- 208
- 209
- 210
- 211
- 212
- 213
- 214
- 215
- 216
- 217
- 218
- 219
- 220
- 221
- 222
- 223
- 224
- 225
- 226
- 227
- 228
- 229
- 230
- 231
- 232
- 233
- 234
- 235
- 236
- 237
- 238
- 239
- 240
- 241
- 242
- 243
- 244
- 245
- 246
- 247
- 248
- 249
- 250
- 251
- 252
- 253
- 254
- 255
- 256
- 257
- 258
- 259
- 260
- 261
- 262
- 263
- 264
- 265
- 266
- 267
- 268
- 269
- 270
- 271
- 272
- 273
- 274
- 275
- 276
- 277
- 278
- 279
- 280
- 281
- 282
- 283
- 284
- 285
- 286
- 287
- 288
- 289
- 290
- 291
- 292
- 293
- 294
- 295
- 296
- 297
- 298
- 299
- 300
- 301










