Featured Blog
-
 May 22, 2026
May 22, 2026By MedStar Team
This article was written by James Howard Street III, MD and Ian Weston, AVP of Operations. A split second can be all it takes for a routine afternoon to turn into a life-altering event. W...
Browse blogs by hospital
Share this
All Blogs
-
August 10, 2017
A “retro” form of pain control is making a comeback in the United States: nitrous oxide, often known as laughing gas. Nitrous oxide was used to ease the pain of labor since the early 1900s. It fell ou...
-
 August 09, 2017
August 09, 2017Clinics Offer Treatment Options Not Widely Available At MedStar Good Samaritan Hospital, one of our main goals is to help you take charge of your health so you can get the most out of life. That...
-
 August 08, 2017
August 08, 2017It’s August—the height of summer—and many of us are taking advantage of the longer days to cram in more outdoor activities. For many, it just seems easier, and definitely more enjoyable, to go for an ...
-
 August 07, 2017
August 07, 2017The Centers for Disease Control and Prevention (CDC) reports that 22.1 percent of adults in Washington, D.C., are obese. Though that’s lower than the national obesity rate of 36.5 percent, it still me...
-
 August 04, 2017
August 04, 2017By MedStar Health Research Institute
Pediatric and Adolescent Gynecology for the Primary Care Provider 2017—Oct. 6, 2017 Pre-pubertal and adolescent girls can experience a myriad of gynecologic problems. Most of these issues can be safel...
-
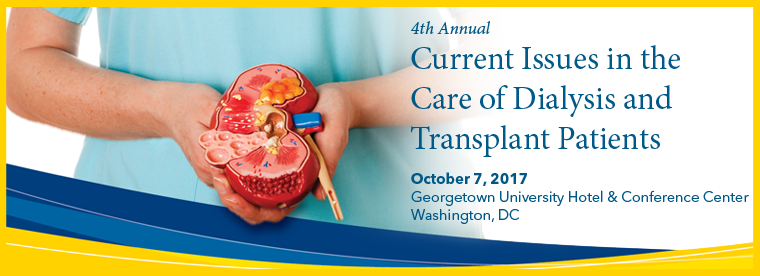 August 04, 2017
August 04, 2017By MedStar Health Research Institute
This one-day educational symposium will examine kidney and pancreas transplantation, with an emphasis on the multidisciplinary approach to pre- and post-transplant care. The conference will provide up...
- 1
- 2
- 3
- 4
- 5
- 6
- 7
- 8
- 9
- 10
- 11
- 12
- 13
- 14
- 15
- 16
- 17
- 18
- 19
- 20
- 21
- 22
- 23
- 24
- 25
- 26
- 27
- 28
- 29
- 30
- 31
- 32
- 33
- 34
- 35
- 36
- 37
- 38
- 39
- 40
- 41
- 42
- 43
- 44
- 45
- 46
- 47
- 48
- 49
- 50
- 51
- 52
- 53
- 54
- 55
- 56
- 57
- 58
- 59
- 60
- 61
- 62
- 63
- 64
- 65
- 66
- 67
- 68
- 69
- 70
- 71
- 72
- 73
- 74
- 75
- 76
- 77
- 78
- 79
- 80
- 81
- 82
- 83
- 84
- 85
- 86
- 87
- 88
- 89
- 90
- 91
- 92
- 93
- 94
- 95
- 96
- 97
- 98
- 99
- 100
- 101
- 102
- 103
- 104
- 105
- 106
- 107
- 108
- 109
- 110
- 111
- 112
- 113
- 114
- 115
- 116
- 117
- 118
- 119
- 120
- 121
- 122
- 123
- 124
- 125
- 126
- 127
- 128
- 129
- 130
- 131
- 132
- 133
- 134
- 135
- 136
- 137
- 138
- 139
- 140
- 141
- 142
- 143
- 144
- 145
- 146
- 147
- 148
- 149
- 150
- 151
- 152
- 153
- 154
- 155
- 156
- 157
- 158
- 159
- 160
- 161
- 162
- 163
- 164
- 165
- 166
- 167
- 168
- 169
- 170
- 171
- 172
- 173
- 174
- 175
- 176
- 177
- 178
- 179
- 180
- 181
- 182
- 183
- 184
- 185
- 186
- 187
- 188
- 189
- 190
- 191
- 192
- 193
- 194
- 195
- 196
- 197
- 198
- 199
- 200
- 201
- 202
- 203
- 204
- 205
- 206
- 207
- 208
- 209
- 210
- 211
- 212
- 213
- 214
- 215
- 216
- 217
- 218
- 219
- 220
- 221
- 222
- 223
- 224
- 225
- 226
- 227
- 228
- 229
- 230
- 231
- 232
- 233
- 234
- 235
- 236
- 237
- 238
- 239
- 240
- 241
- 242
- 243
- 244
- 245
- 246
- 247
- 248
- 249
- 250
- 251
- 252
- 253
- 254
- 255
- 256
- 257
- 258
- 259
- 260
- 261
- 262
- 263
- 264
- 265
- 266
- 267
- 268
- 269
- 270
- 271
- 272
- 273
- 274
- 275
- 276
- 277
- 278
- 279
- 280
- 281
- 282
- 283
- 284
- 285
- 286
- 287
- 288
- 289
- 290
- 291
- 292
- 293
- 294
- 295
- 296
- 297
- 298
- 299
- 300
- 301










